Mouthing off: Most medical schemes ignore the advice that if they provide adequately for oral health
“We are seeing dentists going under,” said Maretha Smit, chief executive officer of the South African Dental Association (Sada).
“Dentists are losing their practices left, right and centre because of the unsustainability of the current model.”
At present, funding private dental health and treatments falls under the ambit of a medical scheme but, according to Sada, oral health benefits for members have been decreasing year on year.
“Medical schemes many years ago provided quite extensively for oral health. Over the years, what’s happened is they have taken the oral health benefit out of the risk pool of schemes and put it in your day-to-day benefits,” she said.
Members’ day-to-day benefits, which are often in the form of a savings account – a portion of their own contribution they have to ration over a period of a year – need to cover, among other things, over-the-counter medicine and general practitioner visits, said Smit.
“That means dentist visits or procedures need to compete in terms of share of wallet with all these other things, meaning patients often neglect their mouths.”
Dental tariffs
A 2004 Competition Commission ruling prohibited medical organisations from determining the pricing of services among themselves because, said the commission, it would amount to collective bargaining or price fixing. This meant medical schemes started to set their own tariffs for services.
“Before this, we set pricing ourselves – taking into account all the overheads associated with modern dentistry and made a scientific calculation. Now we are at the mercy of schemes that cover for dental procedures at woefully inadequate rates,” said Smit.
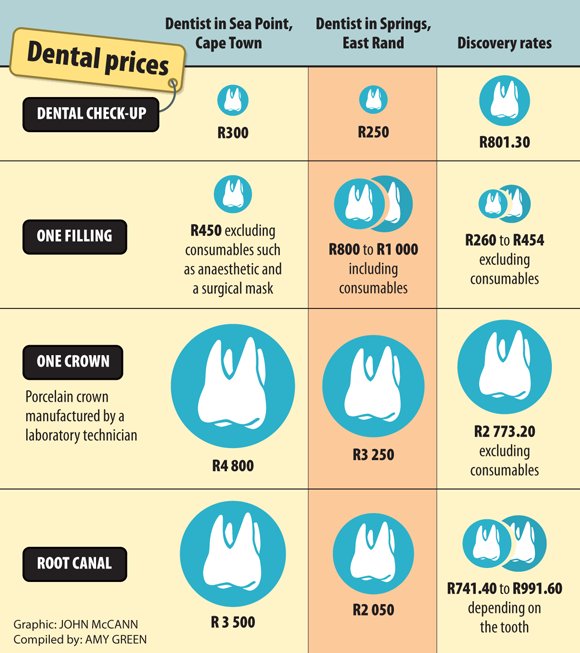
For example, a porcelain crown procedure, during which a tooth-shaped cap is placed over a damaged tooth, manufactured by a laboratory technician, costs R4 800 at one dental practice in Sea Point, Cape Town, and R3 250 at a dentist in Springs on the East Rand. Discovery Health, the largest open medical scheme in South Africa, reimburses up to R2 773.20 from a member’s saving account, excluding consumables like anaesthesia and the sterilisation of instruments.
Smit pointed out that medical savings accounts are often barely able to cover such large amounts – one such dental procedure a year could deplete a member’s account and they would have to pay out of their own pocket for over-the-counter medicine and doctor visits for the remainder of the year.
On one of Discovery’s cheapest plans, the Essential Delta Saver, members make a monthly contribution of R1 252 and have an annual savings account amounting to R2 256 – not enough to cover even one crown. On the other end of the scale, however, their Executive Plan gives a savings account of R12 300 from a monthly contribution of R4 100.
Network benefits
According to the Council for Medical Schemes regulatory body, some schemes do offer plans that provide dentistry benefits outside of medical savings accounts.
“These are typically low-cost and network-based plans that offer a limited day-to-day benefit,” said Daniel Lehutjo, acting chief executive and registrar for the council.
Discovery’s Key-Care plan, the cheapest plan the company offers, is one example that allows patients to consult with a dentist in a network where the scheme has negotiated set prices for reimbursement – usually at cheaper rates because they guarantee the dentist business from members on this plan.
But, according to some dentists, this comes with its own problems.
Adriaan van Niekerk*, a dentist working at Emalahleni in Mpumalanga, is worried that some colleagues, feeling the pressure to attract patients who do not want to make copayments, enter into these network contracts with schemes and, as a result, to “make ends meet”, see as many patients as possible in a day, do their procedures quickly and produce substandard work.
“A lot of my work currently is redoing work of other dentists in the area, who have done a bad job in their haste to see more patients and try to make a profit,” he said. “I spend a lot of time on each patient and make sure I do the procedure properly first time – if I charge medical aid rates for this kind of work, my business will go under too.”
Litigation
According to the nonprofit organisation Dental Protection, the primary insurer for most private dentists in the country, legal cases against the profession have risen in recent years.
“Because of this increased litigation against our profession, our professional indemnity insurance has gone up astronomically. It rose last year by 36%, adding to our already overwhelming list of expenses,” said Van Niekerk.
But Kevin Lewis, director for Dental Protection, said this did not necessarily equate to “diminished levels in the quality of patient care” and could have to do with “increased patient awareness and willingness to raise issues”.
Professional dental insurance is also lower than that for a general practitioner, for example. Van Niekerk pays R5 340 a year whereas general practitioners can pay between R8 000 and R16 000, depending on the procedures they perform in their practices, according to Medical Protection Society, which provides medical professionals with indemnity insurance.
But Van Niekerk argued that a large range of other costs contribute to overheads in dentistry being more expensive than in other medical professions.
Start-up costs
According to Smit, the start-up cost for a “very basic” one-chair practice is about R700 000, excluding the cost of the premises. “A practice with four to five chairs and more sophisticated technology would cost in the region of R6-million.”
According to Mark Sonderup from the South African Medical Association, starting up an extensive general practitioner’s practice can cost “hundreds of thousands of rands” but a basic practice “can probably be established for considerably less than a dentist’s”.
These problems are compounded in less affluent areas where historically patients did not have access to advanced dentistry, according to Thabo Twala, a dentist working in private practice at Mahikeng, North West.
“In the township where I work, people are unable to afford copayments and a lot of them forgo treatment completely because they don’t have any disposable income to pay for medical services,” he said.
“I am seeing fewer and fewer patients because many medical schemes don’t cater for dentistry anymore. Even with the patients who do come, I am experiencing challenges because they don’t have enough dental benefits for me to do all the work they need.”
Smit said the problem is exacerbated by the fact that many South Africans “have a low oral health IQ” and don’t see dentistry as a priority when it competes with other health needs.
“We are increasingly seeing the link between good oral health and good general health – there are strong links between oral health and hypertension, diabetes and heart disease, but many patients are not even aware of this,” she said.
“We are saying to schemes that if they provide adequately for oral health they will save in the long run – but that message is not being taken up.”
Claims refuted
But Alain Peddle, head of research and development at Discover Health, said that there is no evidence to Sada’s claim that dentists are struggling financially, or that many of them are losing their practices.
“In fact, our claims history for the past four years shows a 5% increase in the number of unique practices claiming from us,” he said.
According to Peddle, members of Discovery visit the dentist twice as much as those belonging to other open medical schemes, which is evidence of the success of their “medical savings account” approach and also refutes Sada’s claim that
South Africans have a low oral health IQ.
However, Twala insists the field is in “crisis”.
“In recent years quite a number of black dentists from disadvantaged backgrounds have been graduating, but they find themselves in a situation where they can’t afford to open and maintain dental practices in their communities at all,” he said.
Said Twala: “I realised a long time ago that the situation in dentistry is not going the right way. I’ve got a master’s degree in finance so I can create a second profession for when I can no longer make a living from dentistry. It’s really sad because I love my job.”
*Not his real name
