Keneth Ndua demonstrates his stove invention
A young girl follows her mother down a path that cuts a brown line through the bright green grass as they make their way to their home in the town of Mwingi, 200km from Kenya’s capital city Nairobi. As they approach their home, the girl runs ahead to the man standing in the path. He mirrors her wide smile and laughs at her enthusiasm.
Keneth Ndua is a social entrepreneur. He places a metal stove on the floor as he recounts the story to Bhekisisa.
“That day, it was last year, this young girl told me that since her family started using my stove, she hasn’t missed school,” Ndua says.
“I asked her why and she pointed to her stomach, saying the clean water from the stove doesn’t make her sick with diarrhoea – and she even carries a bottle of water with her to show her classmates. She tells them they don’t need to miss school either.”
In 2008, while working with non-governmental organisations in Nairobi slums, Ndua was struck by the number of people who were ill because of waterborne diseases.
An ongoing health problem
The World Health Organisation (WHO) says cholera, an infectious disease that causes severe diarrhoea, is an ongoing health problem in Kenya.
The most recent outbreak began in December 2014. By May 2015, the disease – caused by the bacterium Vibrio cholera – had killed 65 Kenyans and more than 3 000 people were sick. By this time the outbreak had spread from the Nairobi area to 11 other counties in the country, spurring the government to allocate Ksh500-million ($5.2-million) to cholera control efforts, says the WHO.
In a communique issued by the WHO to address the growing public health emergency, Kenya’s Cabinet secretary for health Jackson Kioko said the disease should not have reached this level because cholera is treatable and can be managed at household level.
Ndua agrees: “I kept wondering, why don’t they just boil the water?”
Back in 2008, he conducted an informal survey among Kenyan women about why they don’t boil water. He found that while some of the women did not have the time to boil water all day, many were concerned about “wasting” their “precious” fire-wood, which they needed to ration for cooking – the fuel was too expensive to do both.
“One lady asked me: ‘If I cannot get enough fuel for cooking, how can you expect me to get fuel for boiling water?'”
Ndua was disturbed by the fact that he could not answer the woman that day and began thinking of possible solutions. “I asked myself what the simplest way to sanitise water is and thought of cooking stoves – there are so many around, everyone has one in their home,” he says.
Back to the drawing board
Ndua asked himself how a cooking stove could solve this problem.
“I went to the drawing board and soon began working on a prototype of a stove that boiled water the same time as you cook,” he explains.
Almost five years later, and after countless attempts using different designs and materials, Ndua’s hard work paid off.
He established his company, Stamp Investments, and received funding for his project in 2013 from the Canadian government, which enabled him to start manufacturing the stove. He named it Jiko Kenya (Jiko is the Kiswahili word for stove or kitchen).
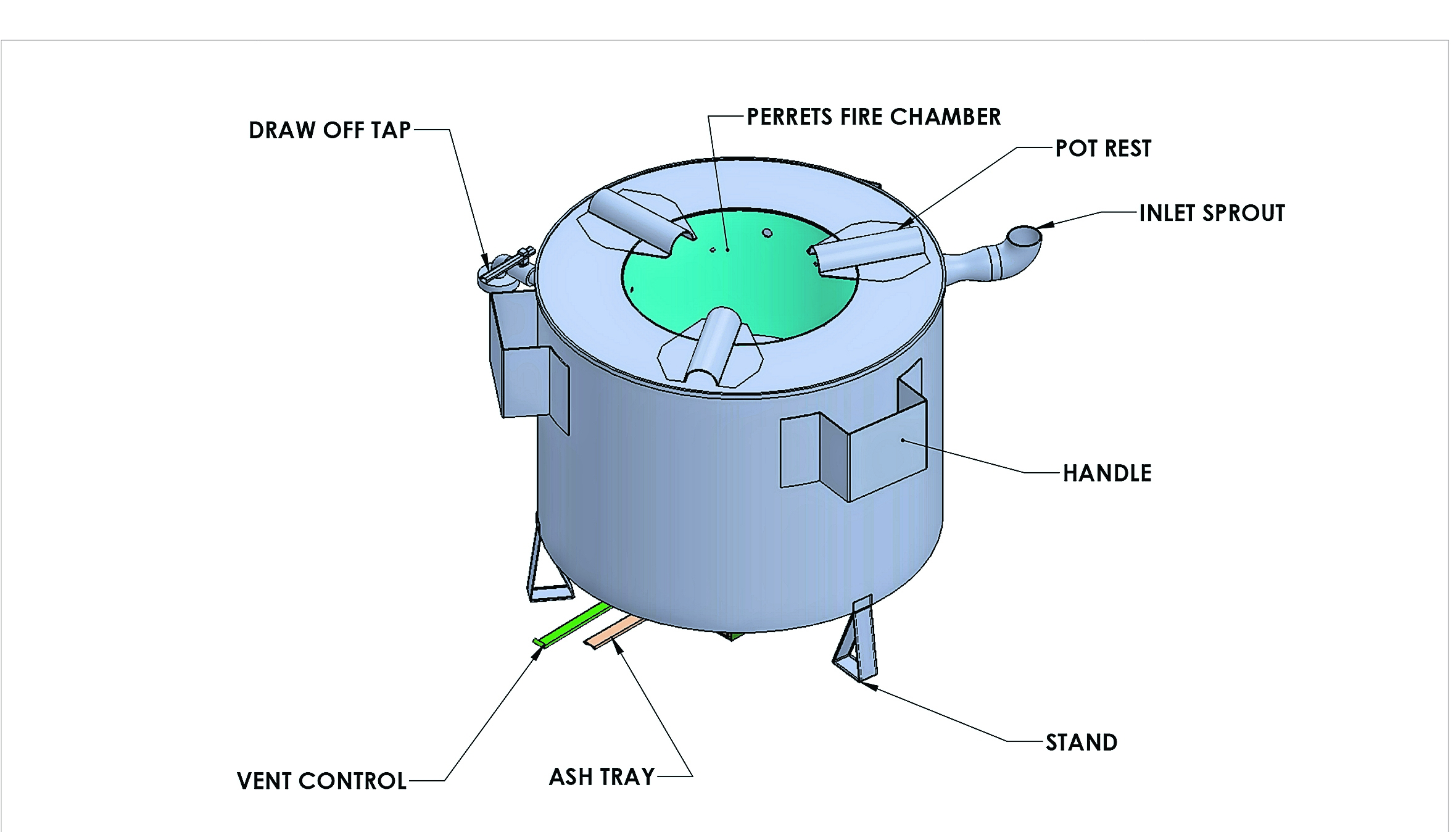
The stove, a small round metal appliance, has two chambers instead of the usual one for firewood. The second chamber holds three litres of water and is insulated from the rest of the device. This means people use the same amount of firewood they ordinarily use for cooking but it also boils water. After 15 minutes, the water is hot enough to kill micro-organisms which cause disease.
Ndua says the clean water is easy to use because there is a tap beneath the chamber. “You continue cooking and pour more water, and on and on, so you have more than enough clean drinking water for the family, and even neighbours, at no extra cost,” he says.
Conducting surveys
As part of the grant funding, Ndua had to conduct surveys to see whether the stove was helping improve the health of the people who used them.
“Between our 2013 baseline survey, and our follow-up survey in 2014, among those who were using the stove there was a massive 70% decline in waterborne diseases,” he says.
The survey was conducted among 65 households in the counties of Kitui, Kiambu and Kilifi who were given the stoves for the purposes of the study.
“It also reduced the costs of going to health centres for treatment in relation to waterborne related sicknesses,” Ndua adds.
Two thirds of the study’s respondents in Kiganjo village in Kiambu county told Ndua and his team that not one family member had fallen ill since they started using the stove.
Ndua has since sold almost 1 000 stoves. He has also managed to bring the actual cost of the stove below those of competitors.
“Our market research showed us a normal stove costs Ksh4 000 ($39) and we are selling ours for Ksh3 000 ($29) and even for less through bulk buying deals,” he says. “People are shocked at the price actually – I have been asked many times if it’s Ksh10 000 or more and then I get to smile when I tell them it’s less than half that.”

After sales service
Ndua and his team regularly return to the study’s households to see whether they are still functioning.
“Because it’s a new product we don’t know how it will work in the long-term so we take a sample stove and open it up back at our facility to test everything is still safe,” he says.
Ndua has received orders from all over the country and is trying to meet the demand – and complete his MBA.
“For other African social entrepreneurs, my advice is to keep looking for solutions to the many problems you see right in front of you and, most of all, don’t give up after a set-back,” he says. “I have seen how something so simple can have a very big impact and if I had given up during my many setbacks I would not be where I am today.
“That’s my story.”
Deconstructing science: What journalists want
[multimedia source=”bhekisisa.org/multimedia/2016-03-03-deconstructing-science-what-journalists-want”]
Waterborne diseases
Cholera and typhoid, two water-borne infectious diseases, are endemic in Kenya, especially in the slums surrounding the capital city, Nairobi, according to the World Health Organisation (WHO).
The country’s largest cholera epidemic to date started in 1997 and lasted until 1999, with almost 35 000 notified cases “representing 10% of all the cholera cases reported from the African continent in the same three years”, says the WHO.
The organisation puts the death toll of the outbreak in 2014 and 2015 at 65, and the number of Kenyans who became ill at more than 3 000.
In Africa, typhoid is most common in Kenya, Nigeria, Mali and Ethiopia, according to a 2008 study published in the Journal of Infection in Developing Countries.
Typhoid is caused by Salmonella enterica and is largely spread through contaminated water sources.
The study notes that there are an estimated 50 cases of typhoid per 100 000 people on the continent each year.
But this is probably an under-estimate because “few studies have been done to confirm the actual number of cases in most of Africa”. For example, the study notes that research done at two Nairobi hospitals reported much higher rates: estimates ranged from 600 to 650 cases of typhoid per 100 000 people annually – mostly in children under the age of 10.
