Lawyers at the lawyers at the Centre for Health
COMMENT
Women often feel forgotten in post-conflict settings, their needs neglected. For them, even seemingly simple ways to prevent HIV transmission present real challenges. Take Cameroon for example, where the average HIV prevalence is 4.3%, according to Cameroon’s Demographic and Health Survey of 2011. In the southwest region, that rate rises to 5.7% but in the post-conflict areas of this region, it could be as high as 20%.
Reach Out Cameroon, a nongovernmental organisation, started a community programme to prevent mother-to-child transmission in the Bakassi area, where decades of conflict between Nigeria and Cameroon over possession of the peninsula only ended in 2008. It has also been doing free voluntary counselling and testing. These tests revealed that while more than 17% of women were HIV positive, the infection rate among men was only 4%.
We know that interventions to prevent mother-to-child transmission of HIV can reduce the risk of infection to less than 5%, according to the World Health Organisation. Normally, the first step would be to get pregnant mothers into healthcare centres to be tested and treated appropriately ahead of the birth, as well as through the process of breastfeeding, if they are HIV positive. But it is not enough to tell women that they must go to a clinic.
Read our story on how programmes on prevention of mother-to-child transmission of HIV impacted on Cotlands baby hospice in Johannesburg.
Limited resources
The high infection rate in Bakassi reflects the real challenges faced by women there: insecurity, no communications network and limited transport. For many women in maritime areas, their only means of transport is by boat – an option that is too expensive to warrant them visiting a clinic. Access is therefore almost impossible and many women end up giving birth to HIV-positive children. This is compounded by the strong influence of culture and religion – many people believe in prayer as an alternative to healthcare.
Culturally, women are reluctant to give birth at an institution if there is a male doctor or nurse present. As a result, many choose to have their babies at home or at a church, using a traditional birth attendant who is unable to provide the necessary support to prevent HIV being transmitted to the newborns. Women’s health choices are further determined by a lack of finances.
Reach Out Cameroon’s programme with the African Women’s Development Fund has found that husbands, who are usually the breadwinners, are more likely to make health decisions about matters such as starting antenatal visits. While the recommended time is 12 weeks into a pregnancy, most women only start having check-ups after 30 weeks – often because of the cost of transport.
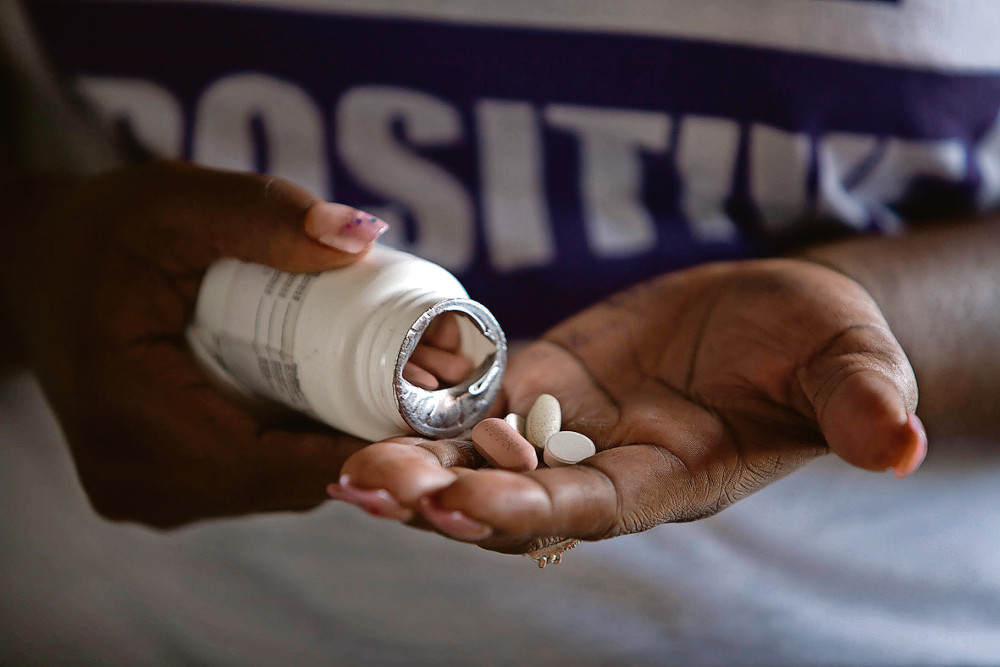
Interventions, such as antiretrovirals, to prevent mother-to-child transmission of HIV can reduce the risk of infection to less than 5%. (Reuters)
Read our story on prevention of mother-to-child programmes in the rural Western Cape in South Africa.
Community health workers
We should not let these women feel forgotten. One solution explored by Reach Out Cameroon is the use of community health workers, as most government health workers don’t operate in these post-conflict areas. The organisation has trained almost 100 community health workers – more than half of whom are women. They, in turn, have reached more than a thousand pregnant women. These workers go from home to home to sensitise residents on the importance of accessing healthcare. They also search for “lost” or lapsed HIV-positive mother-baby pairs to bring them back for care and treatment at the nearest health facility.
Early indications are that about 80% of women reached through this system, and who participated in antenatal care, gave birth to HIV-negative children. This shows a significant reduction of the health burden in a region struggling to contain HIV infections. The results are very promising, but much more can be done. This figure will be even higher if we encourage women to give birth in a medical facility. We have to ensure they have the resources to go to clinics. We also need to find ways for community health workers to go out to assist women who do not want to come to health centres. This might be as simple as doing home-based antenatal consultations where pregnant women get tested and HIV-positive women are treated, followed by regular outreach visits to HIV-positive mother-baby pairs.
Empowering women
Even when women do give birth at home, we need to connect with them to ensure they receive the proper medication. We need an ambulance boat to transport women to the nearest clinic. Women have to be empowered economically so that they can take their own health decisions. We should not let women in this post-conflict area feel forgotten. It is in everyone’s interest that we move this community away from HIV. People move from region to region and having one area with such a high prevalence of HIV puts everyone at risk of infection. If we can make progress in such difficult conditions, we can take lessons learnt to the cities, where such progress can be scaled up quickly and cheaply.
We know that economically empowered women are more likely to take vital health decisions early. We also know that an economically empowered health system is more likely to create an environment conducive to women making these informed decisions. Investing in rural health is critical. The government alone cannot do it – it needs partners in the private sector as well as funders to recognise the economic value of healthcare. If we tackle this now — together— we will make long-term gains.
Ngo Bibaa Lundi Anne is health programme manager at Reach Out Cameroon and an African Women’s Development Fund fellow. Follow her on Twitter @LundiAnne1