The future of our healthcare system is in our hands; we approach it with responsibility, collaboration and a deep commitment to the well-being of all people. (Waldo Swiegers/Bloomberg via Getty Images)
Debate has often portrayed the National Health Insurance (NHI) as being detrimental to South Africa’s already fragile economy — inflicting pain on taxpayers, the public purse and the private sector.
For a country whose growth has more or less stagnated for over a decade, the NHI’s impact on the economy is an important consideration. An insurance scheme that ushers in a better health system could, after all, buoy growth, justifying its existence.
But, as the proposed NHI continues to be stalked by uncertainty, its actual economic pros and cons remain unclear.
The government’s most recent impact assessment contained vague allusions to how the NHI might contribute to economic growth, citing estimates that a one-year increase in a nation’s average life expectancy can increase GDP per capita by 4% in the long run.
Released in 2019, the impact assessment itself is considered outdated by some given the blow to the economy a year later, from the Covid-19 pandemic.
The assessment does, however, identify a recession — which, for all intents and purposes, South Africa currently finds itself in — as a high-level risk to the funding of the NHI. Said funding, the document notes, will rely on the government’s ability to raise taxes, which may be constrained during economic downturns.
Importantly, the impact assessment recognised that South Africa was already in the thick of a downturn in 2019. Today, the country’s economy is only slightly larger (by about R2 billion) than it was prior to the pandemic, which has been followed up with record levels of unemployment and a cost-of-living crisis.
Some will point out that the United Kingdom’s National Health Service (NHS) was devised in the aftermath of World War II, when that nation was overcome by economic crisis. Since its birth almost exactly 75 years ago, the NHS has faced a number of setbacks, including more than a decade of austerity administered by successive Conservative governments.
But the ability of the UK’s government to pull off universal health coverage amid economic headwinds has done little to ease scepticism about South Africa being able to do the same — thanks in large part to the uncertainty that has accompanied the proposed NHI, a predicament that seems to extend to its economic outcomes.
 (John McCann/M&G)
(John McCann/M&G)
“To think about this issue, you have to come at it from different angles,” said Frederik Booysen, a professor of health economics at the University of the Witwatersrand.
For one, there is the question of financing and the knock-on effects of increasing taxes. Financing, as the 2019 impact assessment implies, becomes more difficult the more fragile an economy becomes.
“But I think the other question that needs to be asked is — if the NHI is to improve health outcomes and access to healthcare — then there are many economic implications,” Booysen said.
“When people receive better treatment, you may avert morbidity. You may also avert death. If you’re going to put an economic value to that, then obviously there might be quite a substantial impact. A healthy population has knock-on effects on growth.”
But, as Booysen points out, there is a big “if” attached to the NHI’s actual ability to improve access to good quality healthcare, and thus the country’s economic prospects. “If the system becomes more fragile and care deteriorates … then, of course the picture becomes quite different than in a scenario in which we are very good at implementing it,” he said.
Development economist Anja Smith noted that the NHI is essentially a financing solution, but is relatively silent on the full extent of health service redesign that will need to take place to achieve better health outcomes.
“And I think that that is where a lot of the concerns of stakeholders are coming from. Because I think that behind the NHI there is almost this idea that more money is likely to lead to better health outcomes, which, considering the state of the country’s public sector, isn’t a given.”
Underlying the questions over the feasibility of the NHI is the fact that healthcare, not only in South Africa, is a scarce resource — which, insofar as the public sector is concerned, is also dogged by inefficiencies. This scarcity is partly the result of inadequate spending in the sector.
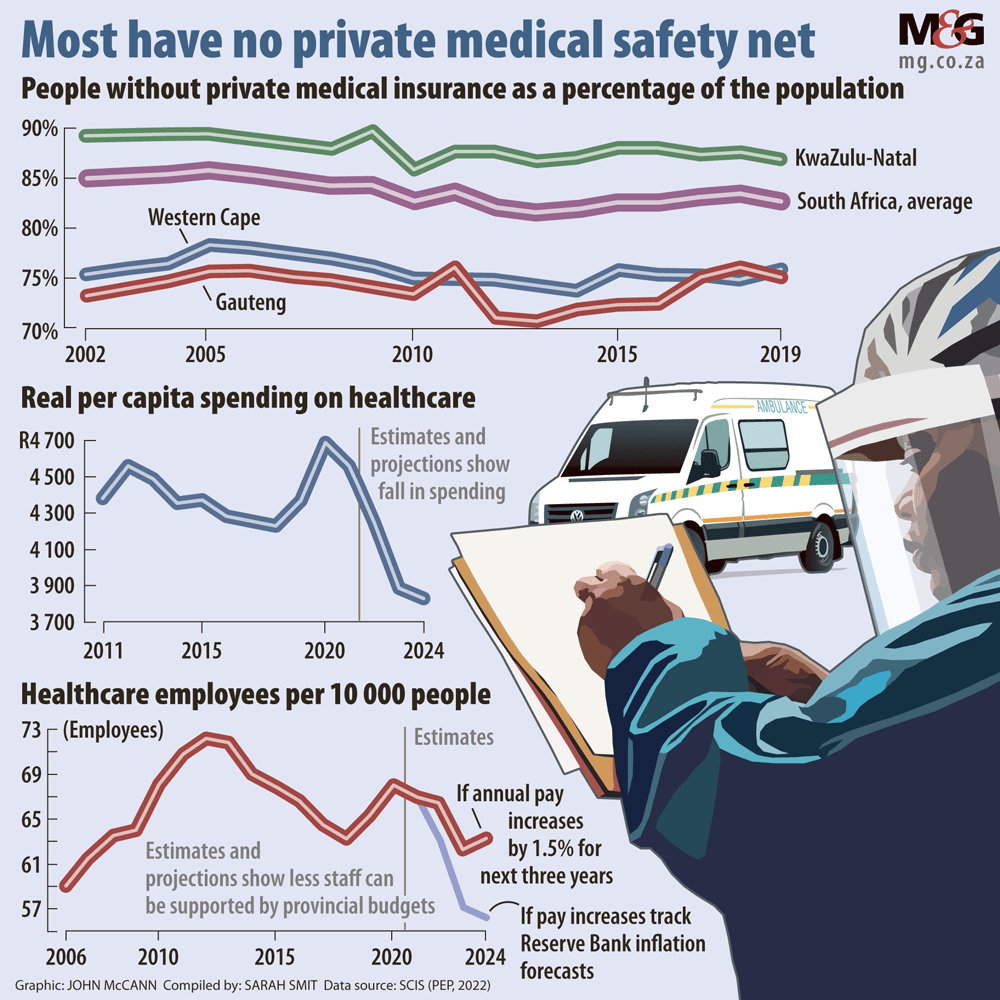
A paper by the Wits University’s Public Economy Project, released last October, estimated that real expenditure per capita on healthcare stagnated between 2011 and 2019, before it was ratcheted up in response to the Covid-19 pandemic.
Referring to the treasury’s spending plans at the time, the paper noted that real expenditure per capita by provincial health departments is projected to fall below its pre-pandemic level over the medium term.
But, in explaining the health system’s failures, experts have pointed to its inefficiencies — rather than to underinvestment alone. “Yes, there is a need for more resources. I do think we’re under-resourced,” Booysen said.
“But, at the same time, if we’re going to put more resources into that pool, we’re going to have to make sure that it makes the biggest difference and that it is spent efficiently
South Africa, Smith said, is likely already spending enough to achieve better health outcomes than it currently is. “So to me, it points to organisational inefficiencies. And the big question is, has the NHI been conceptualised in a way that solves those problems? I think there are big questions around that.”
The uncertainty surrounding the proposed NHI makes it a difficult sell to stakeholders, opening it up to legal challenges that will further delay its implementation. The NHI has been mooted for nearly three decades and, in that time — as unemployment has risen and economic activity has stagnated — the uninsured population has grown faster than the general population.
All there is now are vague claims, often lobbied by disgruntled stakeholders and political parties, about the long-term impact of the scheme — many of them negative. “Things now are anecdotal. It is not based on more rigorous evidence … There are so many unanswered questions that it’s actually frightening,” Booysen said.
“And I think that is the problem with many citizens, many people in the private sector and many healthcare professionals. There is just so much uncertainty.”
That said, the status quo cannot continue — and the NHI provides a good chance to get to the heart of some of the health system’s failures.“It’s a time of uncertainty. But it is also an exciting time. It’s an opportunity to see how we can improve the system — how we can improve on what we have,” Booysen said.
“Some form of NHI may help us get there. We can’t just have a grand vision, a political tickbox, and then nothing happens. So it’s also about everyone holding government accountable to that promise.”