Research shows that drug-resistant TB accounts for a quarter of the 10-million deaths that might be associated with antimicrobial resistance by 2020.
COMMENT
Recently, the United Nations held its first-ever high-level meeting on TB. At the gathering, leaders agreed to treat 40-million people with TB between 2018 and 2022. Heads of state also pledged to ensure that at least 30-million people at high risk of developing TB receive the medication needed to prevent it.
Simultaneously, leaders gathered at the United Nations to take stock of progress made in the fight against non-communicable diseases (NCDs) since adopting a similar declaration to prevent and treat diseases such as mental illness, cancer and diabetes, which often contribute to the spread of TB.
With more than 880 new TB infections and 718 deaths from NCDs daily in South Africa, we need to act with a greater sense of urgency. It is for this reason that Health Minister Aaron Motsoaledi first mooted a UN TB meeting when the body convened a similar summit on antimicrobial resistance.
Rising resistance to common antibiotics, for instance, couldn’t be tackled without addressing TB, he argued. Drug-resistant TB accounts for a quarter of the 10-million deaths that might be associated with antimicrobial resistance by 2020, a 2016 research review found.
South Africa’s call was backed by a number of countries and the UN agreed. We went on to give significant input into the final UN TB declaration, such as insisting that clauses affirming the rights of countries to challenge medicine patents for the good of public health were included. These rights are enshrined in the Doha Declaration and the Agreement on Trade-Related Aspects of Intellectual Property Rights (Trips) and ensure that public health interests supersede intellectual property rights.
 South Africa’s President Cyril Ramaphosa was the only head of state of a Brics country who attended the UN’s high-level meeting on TB in New York.
South Africa’s President Cyril Ramaphosa was the only head of state of a Brics country who attended the UN’s high-level meeting on TB in New York.
But are high-level meetings useful and should we take them seriously? The UN is the world’s Parliament and the most significant instrument for multilateralism. It is expected that the consensus positions adopted by its member states should be implemented.
The TB declaration’s goals are not comprehensive, but they do focus on some of the challenges that have made TB the killer it is. The infectious disease has claimed more lives in the past 200 years than the plague, polio, influenza, cholera, malaria, Ebola and HIV combined, as a piece published in the journal Nature shows.
In the declaration, the world commits to accelerating research and innovation efforts to deliver the first new TB vaccine in almost a century. Recently, we took an important step towards this when South African and international researchers announced in the New England Medical Journal that an experimental vaccine decreased new TB cases by almost half in those who received it.
In New York, we also vowed to leave no one behind, paying special attention to the poor, vulnerable and marginalised, who have always shouldered the heaviest burden of TB because of factors such as poor nutrition and living conditions. The UN’s own secretary general will have to report back in 2020 on whether countries are living up to their promises.
Similarly, the September 26 high-level meeting on NCDs hoped to chart the progress of member states on 22 action-oriented commitments set down in a 2011 UN gathering and accompanying declaration. Three years later at a follow-up meeting, countries pledged to create national targets aimed at treating and preventing burgeoning NCD epidemics.
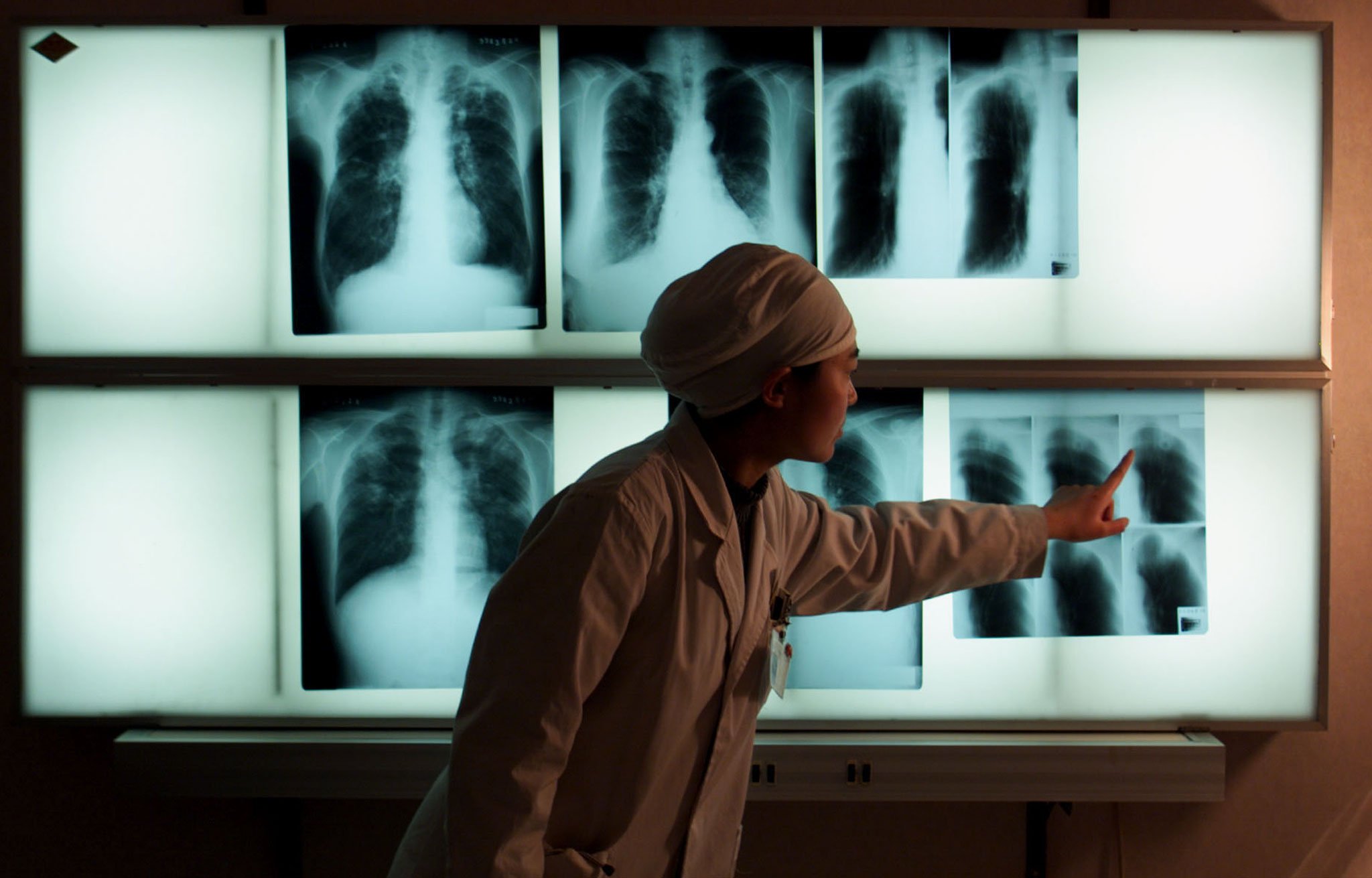 South Africa has more than 880 new TB infections each day, according to the World Health Organisation’s TB report.
South Africa has more than 880 new TB infections each day, according to the World Health Organisation’s TB report.
Every $1 (R15) spent on preventing NCDs brings about a sevenfold return on investment, government officials heard at the high-level UN meeting.
But there has been limited progress since 2014 in reducing deaths from NCDs. It is estimated that more than half of all countries will fail to reach the 2030 NCD targets of reducing premature deaths by one-third from such diseases.
South Africa is one of them.
Watch: Data-driven TB: Using the numbers to find SA’s missing patients
The latest NCD political declaration to come out of the UN at the recent meeting is not much different from those that preceded it. In fact, after reviewing drafts many, including national health department officials, think eight key issues should be at the fore. These include a greater focus on political will and the commercial determinants of health, or the ways in which private sector companies promote products and choices that negatively impact people’s health. We also suggested that there be greater attention to accountability — particularly the creation of an independent body to monitor progress.
There is little new in the 2018 declaration on NCDs apart from the focus on the full implementation of the Framework Treaty on Tobacco Control, which asks countries to ban public smoking. Also novel are references to the private sector’s role in regulating itself.
The NCD declaration’s approach has been criticised as focusing on “lifestyle diseases” in ways that attribute NCDs to individuals’ inability to control themselves by, for instance, “choosing” to eat poorly. In doing so, it’s been accused of downplaying the social and economic contexts that often make it difficult for people to afford to eat healthily, or to resist the marketing of alcohol and tobacco products, etcetera.
So how should South Africa react to these political declarations? President Cyril Ramaphosa considered the high-level meeting on TB important enough to attend and to speak.
He was the only Brics (Brazil, Russia, India, China and South Africa) head of state to do so, despite the fact that Brics countries account for 40% of the world’s drug-susceptible TB cases and half of those resistant to common TB drugs, according to the latest TB report by the World Health Organisation (WHO).
In committing to implementing the declaration, Ramaphosa concluded his remarks by saying: “Please be assured of our commitment to ensuring that we will do everything possible to end tuberculosis as a public health threat by 2030, if not earlier.”
Today, there is already an agreement within the South African National Aids Council that a national meeting will be held to map out our responses.
To do that, we will have to find the third of TB patients who have either never been diagnosed or who have been diagnosed but are not on treatment.
For that, we need mobilised communities that know TB’s symptoms — such as unexplained weight loss and a persistent cough — and can encourage people to get diagnosed and treated as soon as possible. Community health workers, of which there are more than 50 000 in the country, will have to play a bigger role in mobilising communities.
We also need greater investment in research and development including in the search for better vaccines and quicker treatment. More money is also needed to develop new TB tests that can quickly and accurately diagnose people in communities, closer to where they live.
Brics countries are already working towards these goals since the decision to form the Brics TB Research Network was taken in 2016.
With respect to NCDs, South Africa has regulated the use of salt and transfats, as well as tobacco products — and additional regulation is currently being debated.
But over 260 000 deaths were still associated with NCDs in 2016 — nearly 712 every day, Statistics South Africa found.
This may well be an underestimate. We need the recent political declaration on NCDs now more than ever.
The WHO’s 88 “best buys” to deal with NCDs are well researched, including vaccinating girls to prevent cervical cancer, educating people about their risk for NCDs and implementing sugar taxes.
But countries need political commitment at the highest level to implement these and greater regulation of those industries that contribute most to NCDs. The tobacco industry is the only sector that kills its customers, as Uruguay’s President Tabaré Vázquez has said. One may add that this is also true of fast-food businesses and the alcohol industry.
The recent UN meetings on TB and NCDs may have been separate but we must never forget that TB and NCDs are closely related. There are deadly interplays between diabetes and TB as well as alcohol use and the infectious diseases that put both people who drink or who are living with diabetes at an increased risk of developing active TB.
This has major implications for the training of health professionals and how the health system is reconfigured. The health system — and healthcare providers — must, for instance, be able to provide integrated care, or healthcare services that address multiple diseases and risk factors together.
There is clearly much to be done — both by government and civil society — to bring the language of high-level meetings down to the ground and to make sure the promises we made are kept.
Our generation can make a significant difference and history will judge us harshly if we don’t.
Yogan Pillay is the deputy director general for communicable and non-communicable diseases prevention, treatment and rehabilitation. Follow him on Twitter at @ygpillay.