Children's lives are saved in Libya by doctors who can do heart surgery in countries without decent health systems.
A terrified TajAdeen Hussein lay under the blinding lights of the hospital bed. His tiny chest was cracked open, a mess of tubes and equipment protruding from his fragile body.
TajAdeen (not his real name) was only two months old.
Naema Goobha, the head of paediatric cardiology at the Benghazi Medical centre in Libya, retreated from the scene as the surgeon battled to save his life.
In her years of experience, Goobha had never seen a baby in his condition survive.
Libya was ravaged by civil war and its health system collapsing. It made his odds of survival even worse.
Goobha had first diagnosed TajAdeen with a congenital heart defect in the days after he was born. He suffered from a transposition of the great arteries (TGA) with a ventricular septal defect – the two main arteries in his heart were switched in position and there was also a hole between the lower chambers of his heart. His blood was poorly oxygenated, he had blue-tinged skin and was always short of breath.
Research has shown that without corrective surgery, most children with TGA die within six months. “This is one of the types of congenital heart disease that children would be diagnosed with on the first day of their life, and stay with us for one to three months and die before our eyes,” says Goobha.
Soldiers for surgery: How doctors save the lives of war-torn Libya’s children
[multimedia source=”http://bhekisisa.org/multimedia/2016-05-03-soldiers-for-surgery-how-doctors-save-the-hearts-of-war-torn-libyas-children”]
400 babies born each year have heart defects
A 2006 paper in the Libyan Journal of Medicine estimates that between 400 and 600 children are born in the north African country with moderate to severe forms of congenital heart defect each year, and would need surgical or medical intervention in the first year of their life. Because Libya’s health system has virtually collapsed, more recent research is scarce.
TajAdeen desperately needed surgery soon after birth to correct his heart condition but Libya had only one paediatric cardiac surgeon, who operated from a hospital in far-off Tripoli and already had a lengthy surgery waiting list.
In 2014, the year TajAdeen was born, United Nations official Panos Moumtzis told the British Medical Journal (BMJ) that the country was “absolutely being stretched” medically, with a “significant” number of doctors and nurses having left the country.
The World Health Organisation (WHO) said more than 80% of Libya’s nursing staff, many of whom were foreigners, were evacuated that year.
TajAdeen was too ill to consider sending him abroad for surgery. His only hope lay in a humanitarian project run by the William Novick Global Cardiac Alliance, an organisation that provides paediatric heart surgery and training to developing countries in need.
Cardiac alliance steps in
Since March 2012, volunteer cardiac surgeons, nurses and other specialists have made 16 trips to Libya to perform lifesaving surgery on babies and children, and to train local medical personnel.
The team includes surgeons, anaesthetists, nurses, perfusionists to run the heart lung machines, intensive care specialists, a respiratory therapist and often a biomedical engineer whose job it is to ensure the hospital medical equipment doesn’t break down.
The cardiac alliance mentors and trains local health workers to continue to perform the specialised surgery when the team has left. “In the operating room, in the intensive care unit, diagnostic laboratories, our people work side by side with their Libyan counterparts,” says paediatric surgeon William Novick, who founded the cardiac alliance.
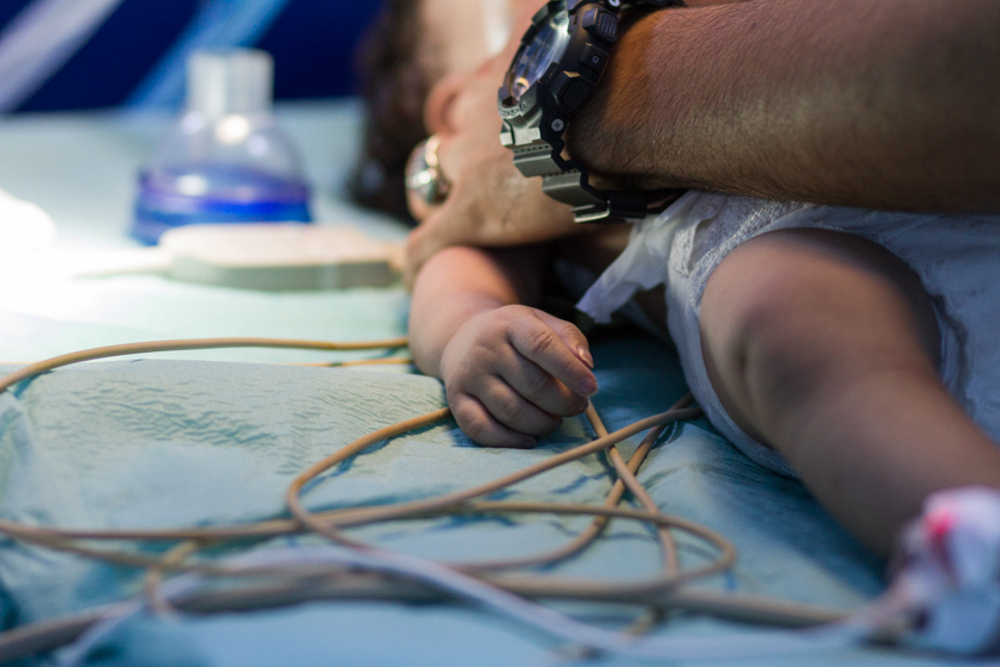
Doctors perform life-saving heart surgery on a child in a Libyan hospital. (Photo: William Novick Cardiac Alliance)
The local team is now able to operate on and care for the more simple cardiac defects.
Wejdan Abo-Amer has been training with Novick’s team for over two years. “When we’re not actually there, she’s operating independently on some of the simpler defects,” Novick says. “Without a doubt she will be a successful, independent paediatric cardiac surgeon in the not too distant future.”
But unless there are more cardiologists on hand to diagnose and operate on babies with congenital heart defects soon after they are born, many will still die.
“The number of children born with surgically correctable heart disease is probably three or four times the number that can be operated on at the Tripoli Medical Centre. Kids are literally just dying, waiting for surgery,” says Novick.
Almost two million in drastic need of help
The WHO estimates that 1.9-million people in Libya require urgent health assistance and this year seeks to raise $50-million for primary health care, essential medicines and to prevent the health system from collapsing.
WHO spokesperson Dr Syed Jaffer, speaking at a briefing earlier this year, said Libyans cannot afford to wait for a political solution. “We need to act now … This is not about politics, it is about health needs.”
At two months, TajAdeen’s surgery was risky – it is safer to perform TGA surgery soon after birth. But Goobha pleaded for him to have the surgery nonetheless.
“I told Dr Novick, ‘If you do only this case, it will be enough for me, I will not ask you to do anything else, ‘” she said.
The family and the doctors decided to go ahead with the procedure. Two weeks later, TajAdeen was fighting for his life in the intensive care unit (ICU) and Goobha was steeling herself for the difficult job of telling the parents their baby was unlikely to survive.
But the doors had not yet swung shut behind her when TajAdeen’s father, a serious young man with the dark eyes and a beard, said: “Don’t worry Dr Naema, he will be okay,” he said.
TajAdeen was fortunate. He survived. He spent a month in ICU before being discharged.
Local expertise is growing
More than 350 children like TajAdeen have so far benefitted from the cardiac alliance’s work. Many others with less complicated heart defects have been treated by specialists such as Goobha and Abo-Amer, who have been trained by the alliance.
But the larger problem of how to revive Libya’s health system remains. In January Libya’s health minister, Reida El Oakley, told reporters that up to 70% of the country’s hospitals were “shut down or totally dysfunctional”.
Two years on, Goobha sits in her office at the Benghazi Medical Centre. She’s reading a case file, but then stops. A little boy has pushed open her door.
TajAdeen is now two years old. “He’s very naughty and very beautiful,” Goobha smiles. “It was so special, this case. He was so tiny, so sweet – helpless. He needed somebody to help him.”
