Mammography is a method for early detection of breast cancer.
The taxi arrived at dawn but it could have come even earlier; I’d been awake all night. I was terrified about the day that lay ahead and what it would mean for the rest of my life.
At the hospital I changed into a high-tech gown that would keep me warm during the long hours I’d be unconscious, and my surgeon arrived to do a quick pre-operative check.
It wasn’t until she was at the door, about to leave the room, that my fear finally found its voice. “Please,” I said. “I need your help. Will you tell me one more time: why do I need this mastectomy?”
She turned back to me, and I could see in her face that she already knew what, deep inside, I had felt all along. This operation wasn’t going to happen. We were going to have to find another way.
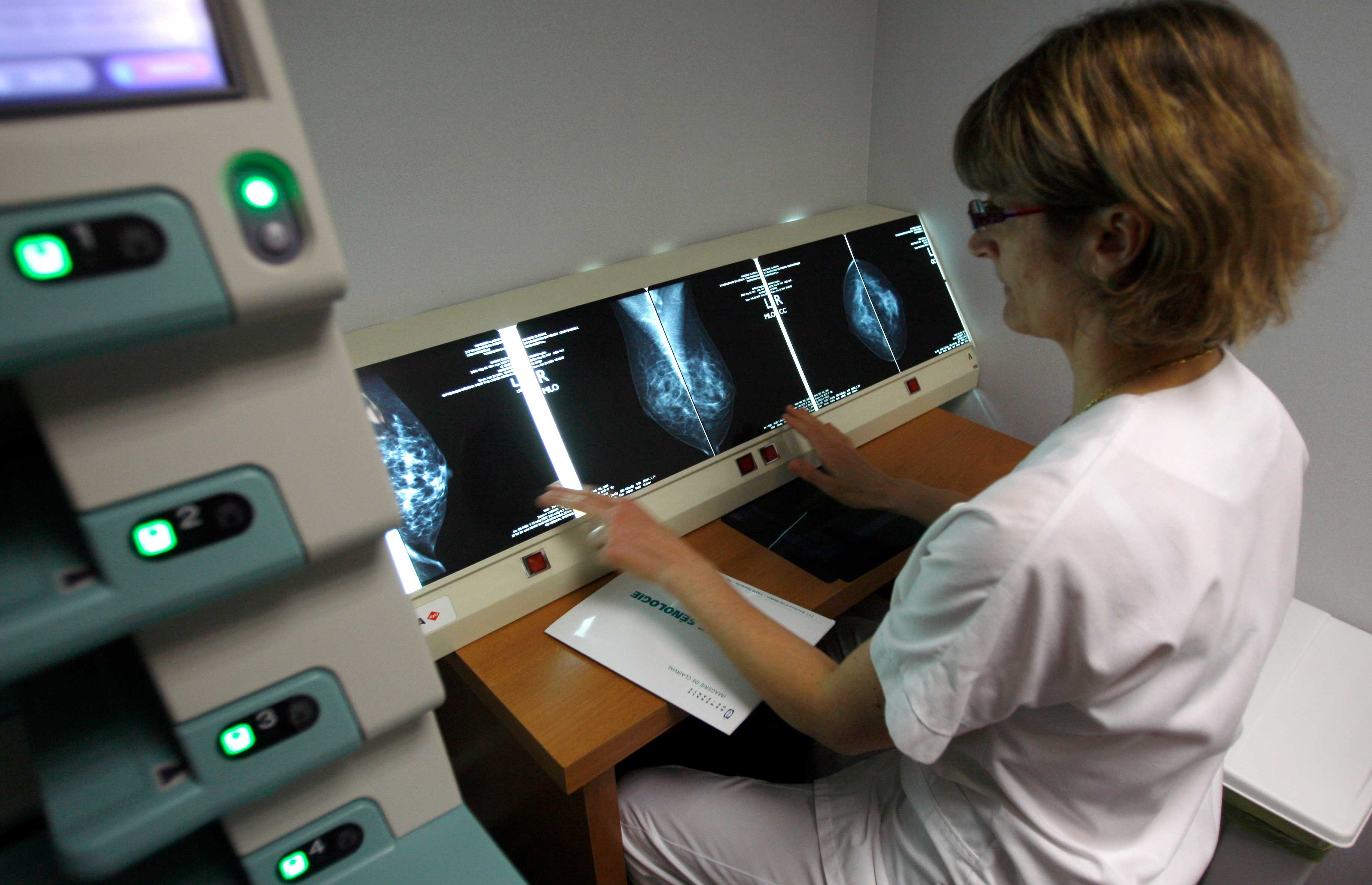 Mammograms may miss some types of cancer and are often used in conjunction with ultrasounds as well as magnetic resonance imaging (MRI) scans to diagnose breast cancer. (Gaetan Bally, Keystone, Corbis)
Mammograms may miss some types of cancer and are often used in conjunction with ultrasounds as well as magnetic resonance imaging (MRI) scans to diagnose breast cancer. (Gaetan Bally, Keystone, Corbis)
Breast cancer had engulfed my life a few weeks earlier, when I noticed a small dimple near my left nipple. The GP thought it was nothing — but why take the risk, she asked cheerfully, tapping on her keyboard to organise the referral.
At the clinic 10 days later, the news seemed optimistic again: the mammogram was clear, the consultant guessed it was a cyst. Five days later, back at the clinic, the doctor’s hunch was found to be wrong. A biopsy revealed I had a grade two invasive carcinoma.
I was shocked, but not devastated. The doctor assured me that I should be a good candidate for what she called breast-conserving surgery, to remove only the affected tissue (this is often called a lumpectomy). That would turn out to be yet another erroneous prediction, though I am grateful for the early hope it gave me. Cancer, I thought, I could deal with. Losing my breast I could not.
The game-changing blow came the following week. My tumour had been harder to diagnose because it was in the lobules of the breast, as opposed to the ducts (where some 80% of invasive breast cancers develop). Lobular cancer often deceives mammography, but it is more likely to show up on an MRI scan. And the result of my MRI scan was devastating.
The tumour threaded through my breast was much larger than the ultrasound had indicated, up to 10cm long.
The doctor who disclosed the news didn’t look at my face; his eyes were fused on his computer screen, his armour against my emotion. We were inches apart but could have been on different planets.
As he began shooting terms like “implant”, “dorsi flap” and “nipple reconstruction” at me, I had not even begun to process the news that, for the rest of my life, I’d have one breast missing.
This doctor seemed more keen on talking surgery dates than helping me make sense of the maelstrom. The one thing I realised was that I had to get away from him. The following day a friend sent me a list of other consultants, but where to start? And then I noticed that only one name on the list was a woman’s. I decided to try and get an appointment to see her.
‘Women have a wide spectrum of feelings about their breasts’
Fiona MacNeill is a few years older than me, in her late 50s. I remember hardly anything about our first chat, just a few days after I read her name. I was all at sea, flailing around. But in the force 10 storm that my life had so suddenly become, MacNeill was my first sight of dry land for days. I knew she was someone I could trust. I felt so much happier in her hands that I had started to blot out the terribleness of losing my breast.
What I didn’t know then is how wide the spectrum of feelings is that women have about their breasts. At one end are those with a take-them-or-leave-them approach, who feel that their breasts are not particularly important to their sense of identity. At the other are women like me, for whom breasts seem almost as essential as heart or lungs.
There is often little or no acknowledgement of this. Most women who have what will be life-changing surgery for breast cancer do not have the opportunity to see a psychologist ahead of the operation.
If I had been given that opportunity, it would have been obvious within the first 10 minutes how desperately unhappy I was, inside myself, at the thought of losing my breast. And while breast cancer professionals know that psychological help would be a big advantage to many women, the sheer numbers of those diagnosed makes it impractical.
The question I wasn’t asking
In many government hospitals in the United Kingdom, where I live, clinical psychology resources for breast cancer are limited. Mark Sibbering, breast surgeon at the Royal Derby Hospital and MacNeill’s successor as president of the Association of Breast Surgery, says the majority are used for two groups: patients considering risk-reducing surgery because they carry gene mutations predisposing them to breast cancer, and those with cancer in one breast who are considering mastectomy of their unaffected one.
Part of the reason I buried my unhappiness at losing my breast was because MacNeill had found a much better alternative than the dorsi flap procedure the other surgeon was offering: a DIEP reconstruction. Named after a blood vessel in the abdomen, the procedure uses skin and fat from there to rebuild a breast. It promised the next-best thing to keeping my own breast, and I had as much confidence in the plastic surgeon who was going to perform the rebuild as I did in MacNeill, who was going to do the mastectomy.
But I am a journalist, and here my investigative skills let me down. What I should have been asking was: are there any alternatives to a mastectomy?
I was facing major surgery, a 10-to- 12-hour operation. It would leave me with a new breast I couldn’t feel and severe scarring on both my chest and my abdomen, and I would no longer have a left nipple (although nipple reconstruction is possible for some people). But with my clothes on, there was no doubt I’d look amazing, with perter boobs and a slimmer tummy.
I’m instinctively an optimist. But while I seemed to those around me to be moving confidently towards the fix, my subconscious was backing further and further away.
Of course I knew the operation was going to get rid of the cancer, but what I couldn’t compute was how I would feel about my new body.
I’ve always loved my breasts, and they’re essential to my sense of self. They’re an important part of my sexuality, and I’d breastfed each of my four children for three years. My big fear was that I’d be diminished by a mastectomy, that I’d never again feel whole, or truly confident or comfortable with myself.
I denied these feelings for as long as I possibly could, but on the morning of the operation there was nowhere to hide. I don’t know what I expected when I finally voiced my fear. I guess I thought MacNeill would turn back into the room, sit down on the bed and give me a pep talk. Maybe I simply needed a bit of hand-holding and reassurance that everything would turn out okay in the end.
But MacNeill didn’t give me a pep talk. Nor did she try to tell me I was doing the right thing. What she said was: “You should only have a mastectomy if you’re absolutely certain it’s the right thing. If you’re not sure, we shouldn’t do this operation — because it’s going to be life-changing, and if you aren’t ready for that change it’s likely to have a big psychological impact on your future.”
It took another hour or so before we made the definitive decision to cancel. My husband needed some persuading that it was the right course of action, and I needed to talk to MacNeill about what she could do instead to remove the cancer (basically, she would try a lumpectomy; she couldn’t promise she’d be able to remove it and leave me with a decent breast, but she would do her absolute best). From the moment she responded as she did, I knew the mastectomy would not be taking place, and that it had been entirely the wrong solution for me.
What had become clear to all of us was that my mental health was at risk. Of course I wanted the cancer gone, but at the same time I wanted my sense of self intact.
A mastectomy might not have to be the only option
Over the three and a half years since that day in the hospital, I have had many more appointments with MacNeill. One thing I’ve learned from her is that many women mistakenly believe that mastectomy is the only or the safest way of dealing with their cancer.
She has told me that many women who get a breast tumour — or even pre-invasive breast cancer such as ductal carcinoma in situ — believe that sacrificing one or both of their breasts will give them what they desperately want: the chance to go on living and a cancer-free future.
That seemed to be the message people took from Angelina Jolie’s heavily publicised decision in 2013 to have a double mastectomy. But that wasn’t to treat an actual cancer; it was entirely an act of prevention, chosen after she discovered that she was carrying a potentially dangerous variant of the BRCA gene. That, though, was a nuance to many.
The facts about mastectomy are complex, but many women undergo a single or even double mastectomy without even beginning to unravel them. Why? Because the first thing that happens to you when you’re told you have breast cancer is that you are extremely frightened. What you’re most scared of is the obvious: that you’re going to die. And you know you can go on living without your breast(s), so you think if having them removed is the key to staying alive, you’re prepared to bid them farewell.
In fact, if you’ve had cancer in one breast, the risk of getting it in your other breast is usually less than the risk of the original cancer returning in a different part of your body.
The case for a mastectomy is perhaps even more persuasive when you’re told you can have a reconstruction that will be almost as good as the real thing, possibly with a tummy tuck to boot. But here’s the rub: while many of those who make this choice believe they are doing the safest and best thing to protect themselves from death and future disease, the truth is not nearly so clear-cut.
“A lot of women ask for a double mastectomy because they think it will mean they won’t get breast cancer again, or that they won’t die of it,” says MacNeill. “And some surgeons just reach for their diary. But what they should do, is ask: why do you want a double mastectomy? What do you hope to achieve?”
And at that point, she says, women normally say, “Because I never want to get it again,” or “I don’t want to die from it,” or “I never want to have chemotherapy again.”
“And then you can have a conversation,” MacNeill says. “Because none of these ambitions can be achieved by a double mastectomy.”
Are South African men more at risk of breast cancer?
[multimedia source=”http://bhekisisa.org/multimedia/2016-11-12-did-you-know-men-can-get-breast-cancer-too”]
Surgeons are only human. They want to concentrate on the positive, says MacNeill. The much-misunderstood reality of mastectomy, she says, is this: deciding whether a patient should or shouldn’t have one is usually not connected to the risk posed by the cancer. “It’s a technical decision, not a cancer decision.
“It may be that the cancer is so big that you can’t remove it and leave any breast intact; or it might be that the breast is very small, and getting rid of the tumour will mean removing most of [the breast]. It’s all about the volume of the cancer versus the volume of the breast.”
‘Double the surgery means double the risks — and it’s not double the benefits’
Breast cancer treatment is becoming more and more personalised. An extremely complex set of variables have to be weighed up that are to do with the disease, the treatment options, the woman’s feeling about her body, and her perception of risk. All this is a good thing — but it will be even better, in my view, when there’s a more honest discussion about what mastectomy can and can’t do.
Looking at the latest available data, the trend has been that more and more women who have cancer in one breast are opting for double mastectomy. Between 1998 and 2011 in the United States, rates of double mastectomy among women with cancer in only one breast increased from 1.9% to 11.2%, a 2015 study published in JAMA Surgery revealed.
An increase was also seen in England between 2002 and 2009: among women having their first breast cancer operation, the double mastectomy rate rose from 2% to 3.1%, a British Medical Journal study found in 2013.
But does the evidence support this action? A 2010 Cochrane review of studies concludes: “In women who have had cancer in one breast (and thus are at a higher risk of developing a primary cancer in the other) removing the other breast (contralateral prophylactic mastectomy or CPM) may reduce the incidence of cancer in that other breast, but there is insufficient evidence that this improves survival.”
“But,” says MacNeill, “double the surgery means double the risks — and it’s not double the benefits.” It’s reconstruction, rather than the mastectomy itself, that carries these risks.
There may also be a psychological downside to mastectomy as a procedure. There’s research to suggest that women who have undergone the surgery, with or without reconstruction, feel a detrimental effect on their sense of self, femininity and sexuality.
According to England’s National Mastectomy and Breast Reconstruction Audit in 2011, for example, only four in 10 women in England were satisfied with how they looked unclothed after a mastectomy without reconstruction, rising to six in 10 of those who had had immediate breast reconstruction.
But teasing out what’s going on for women post-mastectomy is difficult. Diana Harcourt, professor of appearance and health psychology at the University of the West of England, has done lots of work with women who’ve had breast cancer. “Whatever women go through after mastectomy, they tend to convince themselves that the alternative would have been worse,” she says. “But there’s no doubt it has a huge effect on how a woman feels about her body and her appearance.
“Mastectomy and reconstruction isn’t just a one-off operation — you don’t just get over it and that’s it. It’s a significant event and you live with the consequences forever. Even the best reconstruction is never going to be the same as having your breast back again.”
A growing body of mixed research
For much of the 20th century, full mastectomy was the gold-standard treatment for breast cancer. The first forays into breast-conserving surgery happened in the 1960s. The technique made progress, and in 1990, the US National Institutes of Health issued guidance recommending lumpectomy plus radiotherapy for women with early breast cancer. It was “preferable because it provides survival equivalent to total mastectomy and axillary dissection while preserving the breast”.
In the years since, some research has shown that lumpectomy plus radiotherapy might lead to better outcomes than mastectomy. For example, one large population study based in California looked at nearly 190 000 women with unilateral breast cancer (stage zero to three). The study, published in 2014 in the Journal of the American Medical Association, showed that bilateral mastectomy was not associated with lower mortality than lumpectomy with radiation. And both these procedures had lower mortality than unilateral mastectomy.
Research published in the International Journal of Cancer in January, looked at 129 000 patients. It concluded that lumpectomy plus radiotherapy “might be preferred in most breast cancer patients” for whom either that combination or mastectomy would be suitable.
But it remains a mixed picture. There are questions raised by this study and others, including how to deal with confounding factors, and how the characteristics of the patients studied may influence their outcomes.
‘But this much I know: I could not be in a better place’
The week after my cancelled mastectomy, I went back to the hospital for a lumpectomy. I was a privately insured patient. Although I would have likely received the same care on the NHS, one possible difference was not having to wait longer for the rescheduled operation.
I was in the operating theatre for under two hours, I went home on the bus afterwards, and I didn’t need to take a single painkiller. When the pathologist’s report on the tissue that had been removed revealed cancer cells dangerously close to the margins, I went back for a second lumpectomy. After this one, the margins were clear.
Lumpectomies are usually accompanied by radiotherapy. This is sometimes considered a drawback, as it requires hospital visits for up to five days a week for three to six weeks. It’s been linked with fatigue and skin changes, but all that seemed a tiny price to pay for keeping my breast.
One irony about the rising number of mastectomies is that medicine is making advances that are reducing the need for such radical surgery, even with large breast tumours. There are two significant fronts: the first is oncoplastic surgery, where a lumpectomy is performed at the same time as reconstruction. The surgeon removes the cancer and then rearranges the breast tissue to avoid leaving a dent or dip, as often happened with lumpectomies in the past.
The second is using either chemotherapy or endocrine drugs to shrink the tumour, which means the surgery can be less invasive. In fact, MacNeill has 10 patients who have opted to have no surgery whatsoever because their tumours seemed to have disappeared after drug treatment. “We’re a bit anxious because we don’t know what the future will hold, but these are women who are very well informed, and we’ve had open, honest dialogue,” she says. “I can’t recommend that course of action, but I can support it.”
I don’t think of myself as a breast cancer survivor, and I hardly ever worry about cancer coming back. It might, or it might not — worrying won’t make any difference. When I take my clothes off at night or at the gym, the body I have is the body I’ve always had. MacNeill cut out the tumour — which turned out to be 5.5cm, not 10cm — via an incision on my areola, so I have no visible scar. She then rearranged the breast tissue, and the dent is virtually unnoticeable.
I know I’ve been lucky. The truth is that I don’t know what would have happened if we had gone ahead with the mastectomy. My gut instinct, that it would leave me with psychological difficulties, might have been misplaced. I might have been fine after all with my new body. But this much I know: I could not be in a better place than I am now. And I also know that many women who have had mastectomies do find it difficult to reconcile themselves with the body they inhabit after surgery.
What I have discovered is that mastectomy is not necessarily the only, the best or the bravest way to deal with breast cancer. The important thing is to understand as far as possible what any treatment can and cannot achieve, so the decision you make is based not on unexplored half-truths but on a proper consideration of what is possible.
Even more crucial is to realise that being a cancer patient, terrifying though it is, doesn’t absolve you of your responsibility to make choices. Too many people think their doctor can tell them what they should do. The reality is that each choice comes with a cost, and the only person who can ultimately weigh up the pros and cons, and make that choice, isn’t your doctor. It’s you.
This is an edited version of an article first published by Wellcome on mosaicscience.com. It is republished here under a Creative Commons licence.
