Potential white elephant: The construction site of Gauteng’s emergency Covid-19 hospital in Carletonville on the West Rand. It has cost about R500-million, but equipment for patients will add to that. (Paul Botes/M&G)
As the number of new Covid-19 cases in the country declines, the Gauteng department of health is pumping about R500-million into a hospital on the outskirts of Johannesburg that is already more than three months overdue.
According to insiders, the expenditure of half a billion rand is only the start of the project to convert a former mine hospital into a 174-bed intensive care facility. This amount does not include hundreds of millions of rands the state will still have to fork out.
The province must still purchase equipment such as 174 new intensive-care unit (ICU) beds, ventilators, infusion pumps, defibrillators and monitors for each bed. This will drive costs up significantly.
A spreadsheet of Gauteng hospitals’ expenditure on equipment during Covid-19 shows the government paid between R291 000 and R524 000 for a single ventilator, and R86 000 for an ICU patient monitor.
This means that, for the 174-bed hospital, ventilators could cost up to R60-million, and ICU monitors could cost more than R14-million, on top of the R500-million already spent.
A state medical professional with an insider’s understanding of Gauteng health’s hospital network, described the expenditure as a “frenzy”, adding that medical professionals were sidelined in initial discussions. “The prices are a total rip off, and they are still buying.”
Experts and other insiders said that the project — which was initiated in anticipation of an influx of Covid-19 emergency admissions in Gauteng province — is in danger of becoming a white elephant.
Such opaque decision-making is not new. Russell Rensburg, the director of the Rural Health Advocacy Project, said civil society organisations have had a problem with the lack of insight into how the government made decisions about the building and refurbishing of infrastructure during the pandemic.
“The government doesn’t tell us how it decides where they build new health facilities,” he said. “There is a broad consultative process between provinces, and the first point of focus is often the funding, which is defined by a five-year planning framework. “This determines how much will be spent through the health facility revitalisation grant.”.
Funds are allocated to each of the provinces, which decide which projects will be prioritised. Under the disaster-management regulations, command councils took authority and there wasn’t a national plan, Rensburg said. “We should actually have a record of every provincial command council meeting where officials discussed how they made decisions, because after the medium-term budget policy statement, we’re going to be asking for an evaluation of this work over the last six months.”
The project centres on the refurbishment of the AngloGold Ashanti hospital in Carletonville, on Johannesburg’s West Rand. It is part of a R2.5-billion spend by the provincial department of infrastructure development on improving healthcare infrastructure.
This was in anticipation of a chronic shortage of beds in the province’s hospital network at the height of the Covid-19 infections.
When the Mail & Guardian visited the site last week, it was still full of workers from various construction companies, as well as rubble and heavy machinery. The outside work seemed largely complete and teams were working inside.
Despite the sizeable investment and months of working on this project, the Gauteng health department says it is still drafting plans on what will become of the facility post Covid-19. Kwara Kekana, the spokesperson for the province’s health MEC, said the hospital was considered only after all spaces for critical-care beds in existing facilities were used.
“The facility will be reconfigured to address the needs in the region post-Covid, and various options are being considered for the hospital to address the general Charlotte Maxeke cluster-bed needs, considering priority programmes of [the] Gauteng department of health,” Kekana said.
One health professional questioned how the hospital would be integrated into the system, given it is an hour from Johannesburg, and even further from Pretoria.
“Given the chronic shortage of services in hospitals in much more congested areas, it’s still puzzling why so much money has been spent in the middle of nowhere,” said the source.
Gauteng infections peaked in July, when about 3 000 people were testing positive every day. The majority of cases were admitted to private hospitals, according to the National Institute for Communicable Diseases.
On July 7, 3 510 people tested positive. Since then the numbers have declined, and currently about 200 people on average are testing positive for Covid-19 each day in the province. But there is no consensus on whether Gauteng will experience a second wave of infections and, if so, what case numbers could look like.
Prior to the July surge, the department of health had already turned eight facilities into field hospitals, and isolation and quarantine sites, including the Nasrec facility, which was planned to have 1500 beds available including 400 with piped oxygen and 120 with oxygen concentrators.
Kekana said the overall infrastructure expenditure was necessitated by predictive modelling, which indicated a “critical care bed shortage of 2 140 [beds that] needed to be produced”.
“The plan included repurposing of existing beds and spaces in hospitals, [and] additional capacity using alternative building technology structures. There was still a shortfall and a decision was then made to reconfigure the beds at AngloGold Ashanti hospital to close the shortfall,” Kekana said.
Gauteng infrastructure department spokesperson Bongiwe Gambu said the facility was meant to be completed in June, but protests by people associated with local small medium and micro enterprises and a Covid-19 outbreak on site led to a five-week delay.
“Boosting capacity at existing facilities requires decanting and interruption of clinical services, which would delay the delivery of the beds,” she said.
Gambu added that the provincial government has successfully negotiated a 25-year lease for the hospital, at no cost, with Harmony Gold, the buyer of AngloGold’s assets. “The investment is as if we were investing in our own facility and property.”
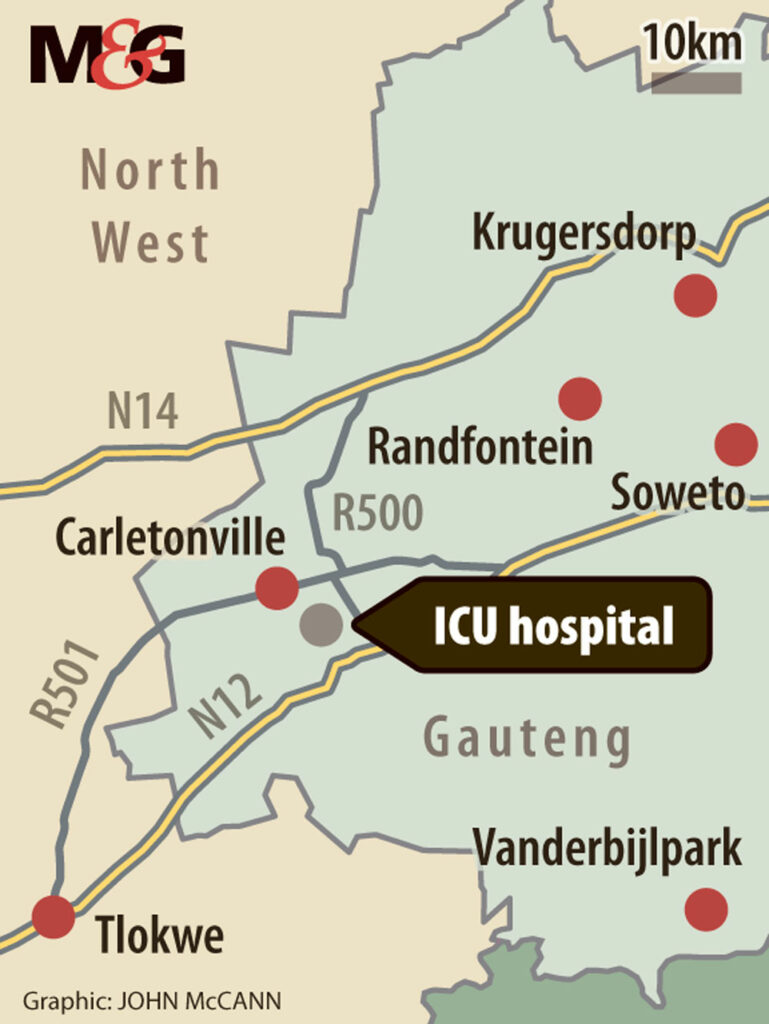 (John McCann/M&G)
(John McCann/M&G)