The demand for donor organs far outstrips the supply because data is not shared, not all hospitals are equipped to do transplants and the National Health Act is inadequate. Photo: Burger/Phanie /AFP
In 2012, at the age of 18 and in matric, Jenna Lowe could barely walk a few steps without collapsing because she frequently ran out of breath.
What was initially thought to be asthma turned out to be a type of blood pressure problem called pulmonary arterial hypertension, which stops oxygen-carrying blood from being delivered to the rest of the body in time.
It is a rare, incurable disease, but a drug called epoprostenol can give a patient some reprieve. The medicine relaxes the blood vessels in the lungs and so makes blood flow easier, which, in turn, puts less strain on the heart to pump out enough oxygen-rich blood.
But this drug wasn’t available in South Africa at the time. Lowe needed an oxygen tank close by and it became so hard for her to move around that she had to get a small scooter to attend her classes at the University of Cape Town.
When her family got her epoprostenol on a compassionate care basis in 2014 (which means South Africa’s medicine regulator allows for a medication that’s not available here to be brought into the country with special permission), breathing got easier — but life didn’t.
The medicine had to be pumped from a small portable device next to her bed so that it could flow directly into the heart uninterrupted 24 hours a day.
 Gabi Lowe (right) had hoped that a pair of lungs would become available to keep her daughter Jenna (left) alive, but she never made it to her 21st birthday after the transplant didn’t work. Photo: Jenna Lowe Trust
Gabi Lowe (right) had hoped that a pair of lungs would become available to keep her daughter Jenna (left) alive, but she never made it to her 21st birthday after the transplant didn’t work. Photo: Jenna Lowe Trust
She needed new lungs. And it soon emerged that a double lung transplant was her best chance of getting back her life.
“We already had a difficult journey by that time, so we thought the transplant would be the easy part,” recalls her mother, Gabi.
With only seven lung transplants having been done in South Africa in 2013, Lowe’s odds of getting new organs were slim.
When someone suffers a bad injury and their brain stops working (called brain death) or their heart no longer beats (called circulatory death), a ventilator can be used to help keep them breathing for a while.
This means organs such as their lungs, heart, liver, pancreas and kidneys can still get oxygen, which keeps them working until the machines are switched off. During this time the organs can be removed for transplanting to save someone else’s life.
In October 2014, Lowe started an online campaign called Get Me to 21, inviting all South Africans to her 21st birthday party on 28 October — on one condition: they had to register as organ donors.
Getting more people to be willing to have their organs go to a new body upon death is only part of the solution to get the supply to match the demand, though.
The transplant chain isn’t working, says Gabi Lowe. “I have so many questions about the system and no one can put it together for me. We need to know what’s happening in the hospitals to understand what’s going wrong.”
Laws of consent
The National Health Act says that from the age of 16 anyone can make it clear that their organs have to be donated by writing it into their will or, with two witnesses present, writing a note and signing it or simply telling someone it’s their wish.
But a medical law expert at the University of South Africa, Magda Slabbert, says “the conditions in the Act are meaningless” because the rules it sets out are not practical.
For example, for a will to be binding, it must be validated by the master of the high court. This can take many days, which, in the case of organ donation can be too long — once the machines have been stopped, a heart should best be transplanted within two hours, while kidneys can stay viable for up to 12.
It’s also not a good idea to keep someone alive artificially (on a ventilator) for too long after their body has shut down, because natural processes kick in after brain death damages organs and so organs need to be harvested before the process has gone too far.
Further, says Slabbert, “signing a document expressing your wishes in the presence of two witnesses makes it a living will, which is not legally recognised in South Africa”.
A living will tells someone’s family only how they’d like their medical affairs to be handled after they die, but the family can override this document because it can’t be challenged in court. And because there’s no central database of such documents, neither a transplant team nor a patient’s next-of-kin can look up a living will and its conditions.
Verbally agreeing that your organs can be donated is also controversial, because it may be difficult to prove that you ever said so.
This means the only way to get permission for taking someone’s organs for donation is by asking the deceased patient’s family, regardless of whether they’re registered organ donors, Slabbert says.
Registering as an organ donor is not legally binding; the same applies to having a sticker on your driver’s licence or an organ donation card in your wallet.
But the Organ Donation Foundation’s registration form still serves a purpose, says executive director of the nonprofit, Samantha Nicholls, because it drives up awareness and creates a record of people’s wishes to be donors.
“We’ve made our database available to all transplant centres, so that the medical team can approach the family with proof of their loved one’s wishes.”
Few donors
In South Africa, donor organs came from less than two out of every million people in 2017. It’s among the lowest donation rates in the world. In Brazil, for example, organs could successfully be given to a recipient from about 16 people per million.
In Spain, a country often noted for having the best legal system for managing donations, almost 47 people per million were actual donors.
In a report from a 2019 workshop co-hosted by the South African Transplantation Society (Sats) and the International Society of Organ Donation and Procurement, experts say having such few actual donations is partly because people’s families don’t agree to it and partly because doctors aren’t referring patients for the process.
When someone has been declared brain dead — after tests by two doctors in the intensive care or casualty unit confirm this — a specialist nurse in charge of the organ donation process at the hospital must be told that there’s a chance for harvesting organs from the body. (The nurse is called a transplant coordinator.)
They must then ask the patient’s family for their permission.
But it’s a difficult decision for families, especially when they’re facing the loss of a loved one.
A 2020 study from the Western Cape shows that in the private sector only about half of the families who were asked to donate their loved one’s organs agreed. In the public sector even fewer families — about a quarter — were prepared to carry out these wishes.
Reasons ranged from families feeling reluctant to make a decision on behalf of someone else to religious and cultural beliefs.
The Sats report notes that, on average, five patients were referred for possible donation a month the year before their survey. This means, on average, only 60 donors got into the transplant chain that year.
In some countries, such as the United Kingdom and Canada, it’s compulsory for doctors to refer patients for organ donation in the event of brain or circulatory death. But this is not the case in South Africa; hospitals without transplant programmes have no obligation to refer patients for organ donation.
There are only 21 hospitals in the country with transplant programmes (11 at state hospitals and 10 in the private sector), and only 26 trained transplant coordinators. At institutions where these roles don’t exist, nurses or junior doctors — without the specific background — have to step in.
David Thomson, a transplant surgeon at Groote Schuur Hospital in Cape Town, says another reason for doctors not passing patients into the system is they don’t have enough information about organ donation.
A 2011 study among medical students at the University of Cape Town found that only about a fifth knew where to find information for potential donors and recipients, and less than 10% were registered donors themselves, because “they had never thought of organ donation” or for religious reasons.
Thomson, who is also the former president of Sats, says new doctors aren’t taught how to talk about organ donation with patients’ families. “If a family doesn’t understand the diagnosis of brain death, they can’t make an informed decision. If you say something careless that will trigger them in the moment, they’re likely to say no.”
No regulations for organ allocations
Because not all hospitals have to participate in the organ donation process, not everyone has the same access to lifesaving transplants.
In the public sector, says Thomson, “there [often] aren’t enough beds in the intensive care unit and hospitals can’t afford the expensive organ support needed [such as dialysis machines] to keep [someone] alive while on the waiting list,” says Thomson. “There is definitely a cost-access problem.”
The World Health Organisation recommends that the government set out transparent rules that define how organs are allocated. But Foster Mohale, the health department’s spokesperson, has confirmed that the state doesn’t have such guidelines and that, instead, provincial and regional committees decide who gets donated organs.
Private and public transplant centres share a waiting list. When an organ such as a heart, lung or liver is donated, it gets allocated based on a points system that considers how long a patient has been in the queue, their age and what the chances are that the transplant will be successful.
Kidney donations are handled slightly differently, and it also depends on the province’s approach. For example, at Groote Schuur Hospital (which also coordinates organ transplants for public hospitals in the Eastern Cape and Northern Cape), the centre from where the donor comes gets one of the pair of kidneys, and the other goes to a patient on the national waiting list.
At Charlotte Maxeke Johannesburg Academic Hospital in Johannesburg, which coordinates organ transplants for other public hospitals in Gauteng, one of the donor’s kidneys goes to a private hospital and the other is given to a public hospital.
Despite this seemingly fair distribution, access to organ transplants isn’t equal between the two sectors.
A report from the South African Renal Registry notes that 54% of kidney transplants were performed in the public sector in 2020, in line with similar trends from Sats data for 2018.
Untangling the collapsed data paints a different picture. In the Western Cape, more than double the donated kidneys went to the public sector; in Gauteng, where most organ transplants are performed, almost 90% of organs went to the private sector — including all livers, lungs and hearts. Only three out of 10 kidneys went to the public sector.
Nationally, seven out of 10 organ recipients were in the private sector.
The department of health does not have its own data or a national register of donors and must rely on other organisations for information. Mohale says the department can’t confirm whether the data is accurate, but that they’re “in the process of taking ownership of statistics in the near future”.
Transplant surgeon at the Wits Donald Gordon Medical Centre and incoming Sats president, Francisca van der Schyff, says the lack of data and transparency surrounding organ allocations reduces the public’s trust in the health system.
She says all hospitals should prioritise organ donation, but points out that it is difficult to motivate why institutions should invest in it without accurate data.
In response to questions about developing a national transplant policy for South Africa, Mohale said there are only “draft regulations on transplants that will cover living and deceased organ donations and allocations”.
Improving organ donation
There’s no magic wand, experts say. But countries around the world are trying to copy Spain, which is considered the gold standard for organ donation. The country has increased donation rates almost 1.5 times since 1989, despite having an ageing population, many patients whose lifestyles push them towards organ failure and less money for a transplant programme than other countries in Europe.
In this country, an opt-out rule applies, which means that everyone is a potential organ donor unless they specifically say that they don’t want to be. But the high donation rate is not simply because of this, write Rafael Matesanz and Beatriz Domínguez-Gil of the Spanish transplant programme, but rather because the focus is on what keeps people from agreeing to donation and working to change perceptions. For example, their national transplant policy focuses on teaching hospital staff to identify potential donors and placing transplant coordinators who are trained to ask for families’ approval in every hospital.
Saying goodbye
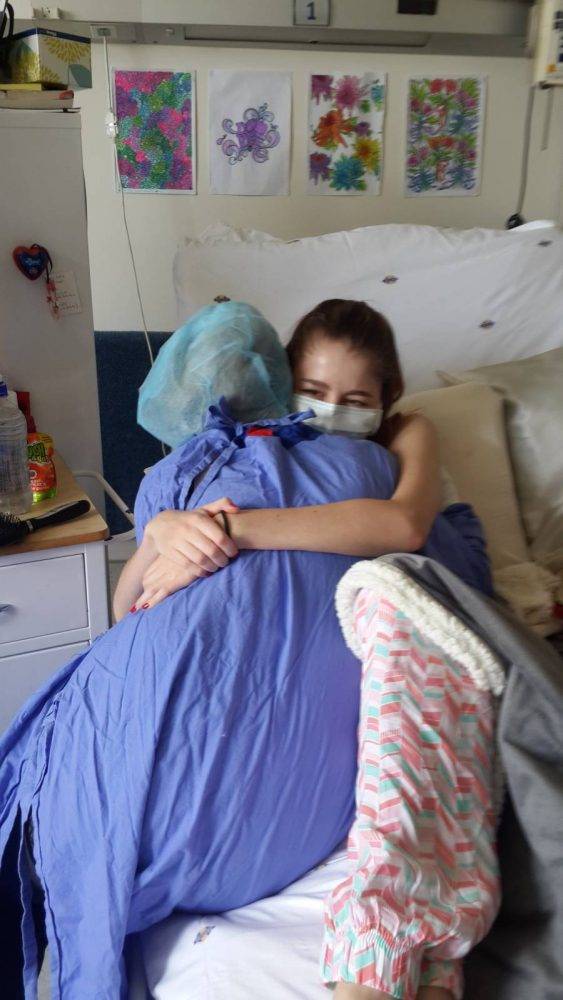 A new breath: Lowe got a lung transplant after waiting more than two years but in the end it was too late. Photo: Jenna Lowe Trust
A new breath: Lowe got a lung transplant after waiting more than two years but in the end it was too late. Photo: Jenna Lowe Trust
On 10 December 2014, the Lowes heard that a pair of lungs had become available and Lowe was air-lifted from Cape Town to a private hospital in Johannesburg.
After the surgery, she had bad seizures and her stomach was paralysed, her mother says. “Jenna couldn’t eat and was being fed through a tube.”
After 185 days in intensive care, her body finally gave in. It was just four months before her 21st birthday.
“I’d fallen asleep by her bed and she reached out her hand and put it on my forehead. She looked at me and said, ‘Thank you, Mommy.’ And shortly after she was gone.”
This story was produced by the Bhekisisa Centre for Health Journalism. Sign up for the newsletter.