Chandre Gould flips to the next Powerpoint slide. “This document was in many ways the Rosetta Stone for the Truth and Reconciliation Commission [TRC],” the security analyst declares. “It was one of the documents found in the trunks confiscated when Wouter Basson was arrested.”
It’s a white stock sheet with four columns detailing items provided to military operatives and security branch members to battle their enemy.
Gould is addressing an auditorium filled with doctors, professors and human rights activists at the University of the Witwatersrand’s medical faculty.
Tonight, June 3, is what doctors here are calling “the eve of Basson’s sentencing hearing”, which is scheduled to take place at the Pretoria offices of the Health Professions Council of South Africa (HPCSA) the next morning.
In December 2013, he was found guilty of unprofessional conduct as a doctor while heading the apartheid government’s chemical and biological warfare programme, Project Coast, from 1981 until 1992.
‘Medically unethical’
The council ruled he was “medically unethical” when he co-ordinated the production of large quantities of illegal psychoactive drugs, equipped mortars with teargas and provided military operatives with disorienting substances to facilitate illegal kidnappings. Basson is also accused of making cyanide capsules available to South African soldiers so that they could commit suicide to avoid revealing information under torture.
The medical ethical principle of “first do no harm” was violated in each instance, the council established.
Basson’s sentencing is a moment many in this auditorium have been waiting for impatiently: the hearing has dragged on for 13 years.
More than 200 registered health professionals, several of them present tonight, and about 30 organisations, including the Black Sash, the Council for the Advancement of the South African Constitution, the social justice organisation Section27 and the HIV advocacy group Treatment Action Campaign, have signed online petitions co-ordinated by human rights group People’s Health Movement, which will be submitted in time for the next day’s sentencing hearing.
“The HPCSA has to take into account in its sentencing the views of the medical community,” says Section27 head Mark Heywood. “We want Basson struck off the medical register forever so he can never again practice as a doctor in South Africa or the world.”
Private practice
This would make it impossible for Basson to continue with his private cardiology practice in Cape Town – one that many of his patients say has saved their lives.
In an email response to the Mail & Guardian, Basson didn’t attach much value to the doings of the movement. “I’ve never heard of the People’s Health Movement and am unaware of any concrete contribution it has made towards the health of South Africa’s population,” he said.
Gould, who now works for the Institute of Security Studies, was one of the TRC investigators in the 1990s who focused on the commission’s chemical and biological weapons warfare programme hearings, in which Basson was a witness.
The trunks with secret military papers were found at the house of one of Basson’s friends. Basson was arrested in January 1997 in a sting operation in Pretoria on charges of fraud and illegal drug possession.
Gould points to the first column on the sheet that would later become known as the notorious verkope lys (sales list).
“What you see are the dates of delivery in the first column. In the second column the products are described,” explains Gould. “Items such as peppermint chocolate brodifacoum, whisky infused with colchicine and bottles of cholera [bacteria]. In the third and fourth columns are the quantities of the products and the prices at which they were sold to police and military operatives.”
Lethal products
The products were intended to kill. Brodifacoum is a lethal rat poison that causes death by thinning the blood so much that the rodents start haemorrhaging. Colchicine is a drug used to treat acute gout but studies have shown that, when high quantities are taken, it can lead to multiple organ failure and eventual death. Cholera is an infectious disease that causes severe diarrhoea and can lead to dehydration and death if untreated. It is caused by eating food or drinking water contaminated with a bacterium called Vibrio cholerae.
Gould says the list was drawn up by André Immelman, the former head of research at Roodeplaat Research Laboratories, one of the front companies established by the military in the 1980s that assisted Project Coast with research by conducting experiments on animals with chemical and biological agents.
The list was used to question Basson in the TRC hearings. It was also used as an exhibit in his 30-month court case that ended in 2002, in which he was found not guilty of human rights abuses, including conspiracy to murder. But, although the court accepted that the list was genuine and these items were distributed to soldiers, it did not agree that it could be proved beyond reasonable doubt that Basson’s intention was to harm people.
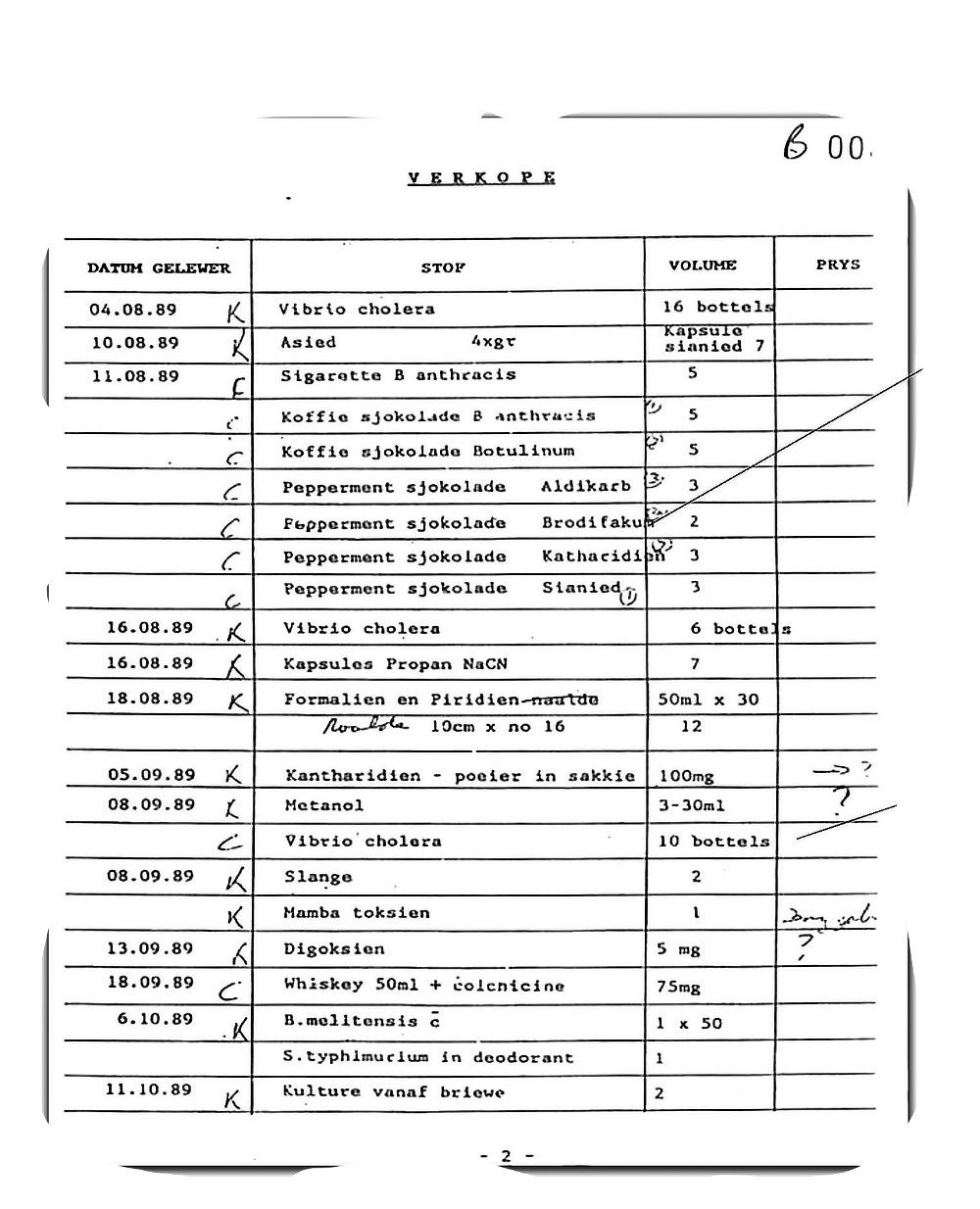
A list of lethal substances provided to military operatives and security branch members.
Basson argued that the items on the document were merely used to train soldiers. Through his lawyers, he told M&G this week: “Everything I did was completely legal under controlled circumstances with the full knowledge and approval of the government of the day.”
But, medical ethics, tonight’s doctors argue, is something entirely different from “what’s legal”.
“What kind of doctor has a shopping list that includes biological toxins?” asks People’s Health Movement chairperson Louis Reynolds. “Basson’s argument that military ethics is different from medical ethics simply doesn’t hold. If he was really simply acting as a soldier, he should have deregistered as a doctor with the council. It’s a problem to switch roles between being a doctor and being a soldier while using the knowledge, skills and privileges of a doctor.”
Anti-fertility vaccine
During Basson’s time as head of Project Coast, there were allegations that he was involved in developing an anti-fertility vaccine for black women. It was never proved in court. But when documentary producer Bob Coen asked him about rumours about his role in creating an “ethnic weapon” known as the “black bomb” for the film Anthrax Wars, which was screened in South Africa in 2009, he responded: “That was great, ja, that was the most fun I have had in my life.”
Basson’s sentencing is a “massive matter with global implications”, warns Heywood. “It’s not a small little thing taking place in the little corner of South Africa.”
Last year a report by the American Taskforce on Preserving Medical Professionalism in National Security Detention Centres found that, after 9/11, health professionals working with United States military and intelligence services “designed and participated in cruel, inhuman and degrading treatment and torture of detainees”.
Heywood says: “If the HPCSA decides not to give the most severe penalty – being struck off the medical roll – it would be a dent in the state of global medical ethics. It would mean that US doctors who may be complicit in torturing detainees in Guantanamo Bay, should they ever be charged with violations of their professional ethics, would be able to cite this precedent: that Wouter Basson got away with it.”
But why should a doctor regarded by some as one of the best cardiologists in the country be barred from practising in a country with a drastic shortage of heart doctors? And this, more than two decades after he acted unethically and after he has run a successful private practice for several years?
Because good technical skills are no guarantee of good ethics, says Heywood.
Cardiologists
According to the South African Heart Association, which represents the professional interests of cardiologists, South Africa produces only six to 10 cardiologists a year. Provinces such as Limpopo, North West and Mpumalanga don’t have a single cardiologist in the state sector, the association’s president, Adriaan Snyders, says.
Heywood responds: “We have a shortage of Paralympians. But if Oscar Pistorius is found guilty of murder, we’re not going to say, we’ve got a shortage of global champions, so let him continue to run.
“We know there is a shortage of cardiologists and that’s tragic. But the solution is for the state to train people rapidly to meet that shortage. The answer isn’t to take people guilty of crimes of his severity [unethical conduct] and ask them to fill that gap.”
Salim Abdool-Karim is one of South Africa’s most renowned HIV scientists and doctors who was the president of the Medical Research Council until recently. He’s the director of the Centre for the Aids Programme of Research in KwaZulu-Natal, which has done ground-breaking work on HIV vaccines and microbicides. He signed the doctors’ petition without the slightest bit of doubt.
“I just don’t buy the point he raised in his mitigation that he has many patients, lots of them black, that will lose him as a doctor if he can’t practice,” Abdool-Karim says. “He has to be held accountable for what he did at that time. He has to pay his debt to society and those who fell victim to his work under apartheid.”
Accountability project
But the Doctors Who Torture Accountability Project, which monitors unethical medical behaviour worldwide, has found that the council doesn’t have a reputation for “systematic punishment of doctors abetting torture”.
Not even the state doctors who treated former Black Consciousness Movement leader Steve Biko, who were both found guilty of unprofessional conduct in 1985, were removed from the medical register.
According to the council’s chief operations officer, Tshepo Boikanyo, Ivor Lang was cautioned and reprimanded for failing to examine Biko properly and Benjamin Tucker was suspended for three months for allowing a semicomatose Biko to be transported naked in chains in the back of a Land Rover from Port Elizabeth to Pretoria. Biko died shortly thereafter.
The HPCSA’s spokesperson, Charmaine Motlaung, could not tell the M&G how many doctors had been removed from the medical register in the past decade or for what offences.
Timely ruling
Many of the doctors and activists in tonight’s audience doubt the council’s ability to come up with an appropriate and timely ruling. It’s partly why they have started the petitions.
According to Heywood, the HPCSA lacks the ability to properly “police the medical profession” and needs “better leadership and more resources to conduct itself better generally”.

Former military psychiatrist Aubrey Levin became notorious for administering electric aversion therapy to gay soldiers.
Basson was found guilty only 13 years after 40 doctors laid a complaint against him – to a great extent because his legal team has managed to endlessly delay his hearing dates. “It’s time for the HPCSA to assert itself now on this matter. They are entitled to for instance meet over a weekend if necessary,” says Heywood. “Thirteen years for the man to be found guilty is ridiculous. How long is it going to take to sentence him?”
Part of the reason why Basson’s colleagues are unsympathetic towards him is because he has never expressed remorse.
“I’m afraid Wouter Basson has never shown any appreciation that what he did was fundamentally wrong. He has been saying he basically couldn’t care,” says Leslie London from the University of Cape Town’s School of Public Health and Family Medicine. London was one of the doctors who laid a complaint with the HPCSA against Basson in 2000.
“Denying what he did was wrong” is the approach Basson would be taking in “the next few days of sentencing hearings as well”, Gould says.
Focal point
But then an audience member gets up and asks: “To what extent is there the danger that this doctor is being made too much of a focal point for unethical behaviour among South African doctors? Are we not distorting the narrative, since there are many others who have not been prosecuted?”
According to London, shortly after Basson’s complaint was submitted to the council, the names of 40 other doctors who were cited in the TRC health sector hearings were submitted to the HPCSA by TRC investigators. When the investigation came to nothing, London resubmitted the names to the registrar of the HPCSA.
One of the doctors on the list was former military psychiatrist Aubrey Levin, who moved to Canada to work as a forensic psychiatrist in the mid-1990s. Levin was notorious for heading a controversial military programme to “cure” gay soldiers with electric aversion therapy. He was jailed in Canada earlier this year after he was found guilty of sexually harassing his patients.
According to reports published in the Calgary Herald, Levin claimed in court that he was merely using treatment techniques he had learned in South Africa.
“Levin escaped justice quite nicely but it eventually caught up with him,” London says. “Unfortunately, the victims of his aversion therapy in South Africa will never get any justice.”
TRC
None of the 40 doctors has been investigated in South Africa and Motlaung could not tell the M&G why not. She confused those doctors with ones who had applied for amnesty at the TRC and, therefore, could not be legally prosecuted.
According to Motlaung, Levin deregistered with the council shortly after he moved to Canada. This would have made it impossible for the HPCSA to prosecute him.
But that is exactly the problem, says ophthalmologist Khosi Lethlape, president of the African Medical Association. South Africa needs a better mechanism to prosecute unethical medical behaviour, in which “doctors are held accountable as members of society”. “All you need to do is to deregister from the council as a health professional and there is nothing it can do,” he said.
London believes the reason unethical behaviour such as that committed by Basson and other health professionals during apartheid was possible because of military and state secrecy. “What went on in Project Coast was because you needed security clearance to get [in] there and, once you were in, it was a totally closed project. These things would not have gone wrong if there was civilian or professional peer oversight in what happens in these high-risk situations.”
But secrecy and silence and their impact on medical ethics, one audience member points out, is not reserved for the military, “wars” or apartheid.
“What about doctors in administrative leadership positions who are presiding over corrupt tenders and maladministration in hospitals? That type of unethical behaviour directly leads to the death and suffering of patients. I look forward to the day when the HPCSA puts the first hospital administrator in front of them to respond.”
Whistle-blowers
Lethlape says whistle-blowers in the health sector are seldom protected. Those who want to prevent what Lethlape terms “medical human rights abuses because of a lack of access to treatment” get victimised.
“Look at Thys Mollendorf,” Lethlape says. He was fired as the superintendent of the Rob Ferreira Hospital in Mbombela in 2002 for allowing an anti-rape project to use a room to provide HIV treatment and counselling before antiretroviral treatment was official government policy during former president Thabo Mbeki’s “Aids denialist” reign.
“It’s all good and well to talk about ethical behaviour. But if doctors work in an environment in which being ethical is not supported or promoted, they’re basically sacrificing themselves. How do we balance those issues?” Lethlape asks.
At 9.07 the next morning, June 4, when most of the Wits audience members were already preparing to follow Basson’s 10am sentencing hearing on social media the next day, the HPCSA sent out the following email notice: “The Health Professions Council of South Africa hereby gives notice of the postponement of the sentencing of Wouter Basson, because of the unavailability of Basson’s legal counsel … A new sentencing date will be announced as soon as it has been set.”
Two weeks later, no date has been set. “Every day of these postponements is an insult,” Heywood says. “It goes against medical ethics.”
